Journal of Nutrition & Food Sciences
Open Access
ISSN: 2155-9600
ISSN: 2155-9600
Expert Review - (2021)Volume 11, Issue 2
Generally our human body contains large number of bacteria, viruses and fungi and they are collectively known as the microbiome community. While some bacteria are associated with disease, others are actually very important for strengthening of our immune system, proper functioning of the body organs including heart, maintenance of body weight and many other aspects of health. Trillions of these microbes exist in our body system particularly in the intestines and skin. Most of the microbes are associated in the large intestine in the form of a pocket called the cecum, and they are referred to as the gut microbiome. Although many different types of microbes are present in our body, however most of the studies have been carried on bacterial composition of the digestive gut system. In fact, there are several reports that the human body contains more number of bacterial cells than the actual human cell counts. It has been estimated that roughly 40 trillion bacterial cells are present in our body whereas human cells counts are around 30 trillion. Scientists all over the world have reported about 1,000 species of bacteria in the human gut microbiome, and each of them plays a different role in the body. Most of them are extremely important for maintaining our body health, while few species may be harmful in creating some serious diseases. Altogether, these microbes may weigh as much as 2-5 pounds (1-2 kg), which is roughly the weight of our brain.
Food and nutrition; Microbiome; Human body
Gut Microbiome Composition
Human microbiome consists of micro-organisms like bacteria, archea, fungi, protozoans, and viruses (Figure 1). Among all microbiome micro-organisms, bacteria are the most predominant and the presence of bacterial population has been estimated between 75 to 200 trillion in a single person. The first bacterium that was noticed in the intestinal region was Escherichia coli in healthy children and in the children suffering from diarrheal disease. Other bacterial species observed were Veillonella parvula in the digestive tract and Bifidobacteria in the intestinal fluid [1]. Later number of micro-organisms has been identified in the human gut system after the discovery of the molecular tools for DNA analysis. It has been estimated that human microbiota consists of more than 1000 different species of micro-organisms. Further it is reported that human gut microbiome contains more than 160 species of bacteria. Besides healthy bacteria, there are number of unhealthy/pathogenic bacteria like Staphylococcus, Streptococcus, Enterococcus, Klebsiella, Enterobacter and Neisseria causing various types of intestinal disorders. Clostridium difficile a pathogenic bacterium most commonly found in the human gut microbiome causes severe recurrent diarrhea. The bacterial species like Prevotella and Firmicutes and their abundant presence in the gut system have been correlated with obesity (Table 1).
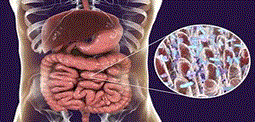
Figure 1. Intestinal microbiome community (Source: internet web).
| S.No | Bacterium found in human colon |
|---|---|
| 1 | Bacteroides fragilis |
| 2 | Bacteroides melaninogenicus |
| 3 | Bacteroides oralis |
| 4 | Enterococcus faecalis |
| 5 | Escherichia coli |
| 6 | Enterobacter sp. |
| 7 | Klebsiella sp. |
| 8 | Bifidobacterium bifidum |
| 9 | Staphylococcus aureus |
| 10 | Lactobacillus |
| 12 | Clostridium perfringens |
| 13 | Proteus mirabilis |
| 14 | Clostridium tetani |
| 15 | Clostridium septicum |
| 16 | Pseudomonas aeruginosa |
| 17 | Salmonella enterica |
| 18 | Faecalibacterium prausnitzii |
| 19 | Peptostreptococcus sp. |
| 20 | Peptococcus sp. |
Table 1: Bacterium found in human colon.
Microbiome Benefits
Microbiome in human body is associated since our birth time onwards and play very important role to carry out various physiological functions. There are also reports that once the baby is born in mother’s womb the baby is exposed to the microbes through mother’s placental cord. However, new evidence suggests that babies may come in contact with some microbes while inside the womb. As the baby grows the gut microbiome of the baby begins to diversify indicating that different types of microbial species start accumulating and it is assumed that more the diversification is good for the health. Later depending on the food we eat affects the composition, quality and diversity of the gut microbiome. Dietary food habits always influence the diversity of the gut microbiome which in turns affects the body functions. For example, Bifidobacteria first begins to grow in the new born babies’ intestine because they very much essential for the digestion of healthy sugars in the breast milk and these sugars are important for growth of the babies. There are certain bacteria which digest the fiber, producing short chain fatty acids and these fatty acids are most essential for the maintenance of gut health. Fiber may also help to prevent weight gain, diabetes, heart disease and the risk of cancer etc. There are several reports indicating that the gut microbiome help in improving the immune system. By communicating with immune cells, the gut microbiome can control our body by developing resistance to the infectious bacteria. In recent years several researchers have found out that the gut microbiome also plays important role in controlling the neurodegenerative disorders like Alzheimer’s disease and Parkinson disorder. Therefore, there are a number of different ways in which the gut microbiome can affect key bodily functions and influence our health. There are several other benefits and few of them are summarized below [2].
Gut microbiome and body weight
Several studies on the composition of microbiome present in our intestinal portion have shown that there are thousands types of different bacteria involved with our body system. The composition analysis indicates the presence of both good and unhealthy bacteria. When there is a dominance of unhealthy microbes in the gut system which is also called gut dysbiosis then there is a possibility of increase in our body weight. Several confirmed studies have shown that the gut microbiome differed completely between identical twins, one of whom was obese and one of whom was healthy. This demonstrated that differences in the microbiome diversity is not genetic related. Interestingly, in one study, when the microbiome from the obese twin was transferred to mice, they gained more weight than those that had received the microbiome of the lean twin, despite both groups eating the same diet. These studies indicated that microbiome dysbiosis may play a role in weight gain [3].
Microbiome and maintenance of gut health
The microbiome present in the gut also plays vital role in maintaining the health of the gut system. This has been confirmed by number of research studies on intestinal microbiome analysis. Unhealthy microbiome create number intestinal disorders like Irritable Bowel Syndrome (IBS) and inflammatory bowel diseases, the bloating, cramps and abdominal pain that occurs due to presence of IBS. This is because the microbes produce a lot of gas and other chemicals, which contribute to the symptoms of intestinal discomfort. However, certain healthy bacteria in the microbiome can also improve gut health. Certain Bifidobacteria and Lactobacilli, which are found in probiotics and yogurt, can help seal gaps between intestinal cells and prevent leaky gut syndrome. These species can also prevent disease-causing bacteria from sticking to the intestinal wall. In fact, taking certain probiotics that contain Bifidobacteria and Lactobacilli can reduce symptoms of IBS.
The gut microbiome and heart health
Several researchers in recent past have reported that the gut microbiome play a very vital role in maintaining the health of heart. Developing healthy microbiome in the gut system has been correlated with production of HDL cholesterol and unhealthy species of microbes present in the gut microbiome community have been correlated with the heart disease by producing tri-methylamine N-oxide (TMAO). TMAO is a chemical that contributes to blocked arteries, which may lead to heart attacks or stroke. Certain bacteria within the microbiome convert choline and L-carnitine, both of which are nutrients found in red meat and other animal-based food sources, to TMAO, potentially increasing risk factors for heart disease. However, other bacteria within the gut microbiome, particularly Lactobacilli, may help to reduce cholesterol when taken as a probiotic.
Gut microbiome and diabetes
The quality of gut microbiome and its influence on controlling blood sugar levels has also been reported by number of workers. Both types diabetes 1 and 2 can be controlled by developing appropriate and healthy gut microbiome. In one of studies in recent years reported that in number of infants who had a genetically high risk of developing type 1 diabetes, these infants have shown less diversity in their gut microbiome composition and the available microbes in the gut system were found to be unhealthy. In another observation it was noticed that people who have unhealthy microbiome community in their gut system, there was a great variation in their blood sugar levels. To confirm this kind of correlation more research studies are needed not only on microbiome composition but also on the microbial ingredients and their chemical identity.
Gut microbiome and brain health
Correlation of functioning of brain and neuro-disorders with the gut microbiome has been carried out by number of investigators. For example certain species bacteria present in the gut system help to produce chemicals in brain called neurotransmitters like serotonin which is an antidepressant. Morphologically the gut is connected to the brain through millions of nerves and therefore, the gut microbiome may also influence brain health by controlling the messages that are sent to the brain through these nerves. It has been reported that the gut contains around 500 million neurons which comprise the enteric nervous system. The interaction of the gut which influences upon the nervous system, and vice versa, is known as the ‘gut-brain-axis and recent evidence suggests that the gutbrain- axis may be implicated in a range of neurological disorders including Multiple Sclerosis (MS), Parkinson’s disease and dementia. It has been observed that there were alterations in the composition of gut bacteria in patients with Alzheimer’s disease compared to healthy controls. For example, Clostridium and Bifidobacterium species were less abundant in Alzheimer’s disease patients whereas Bacterioides and Gemella were more abundant. Furthermore, cerebrospinal fluid markers for Alzheimer’s pathology, such as the levels of amyloid-beta protein, could be correlated with a change in the number of certain bacteria in the gut. It is mentioned that decrease in the number of Bifidobacterium which is known to be reduced in Alzheimer’s could directly be correlated with high levels of amyloid-β-protein in the cerebrospinal fluid of patients with Alzheimer’s. It is mentioned that bacteria that secrete lipopolysaccharides (LPS) and amyloid can trigger profound inflammatory changes within the gut, and therefore within the brain. Inflammation within the gut can cause the gut to become ‘leaky’ as well as causing the Blood-Brain-Barrier (BBB) to become more permeable. As such, inflammatory molecules can enter the brain through a compromised BBB to trigger brain inflammation, which could trigger or exacerbate Alzheimer’s pathogenesis. One such bacterium that may induce neuro inflammation and initiate neuro-degeneration through the gut is Bacterioides fragilis. An accumulation of recent evidence suggests that an imbalanced gut microbiome (dysbiosis) could lead to Alzheimer’s disease and wider neuro inflammation through the gut-brain-axis. Promoting ‘good bacteria’ relative to ‘bad bacteria’ in the gut may be important in maintaining good digestive, immune and neurological health. Our understanding of how certain gut bacteria can influence brain health is a developing field and more research studies are needed so that new drug discoveries can be made for effective therapies [4].
Build up healthy gut microbiome
There are many ways to improve our gut microbiome. Following are few important steps:
• Consuming diverse range of appropriate type of food can lead to develop healthy microbiome, which is an indicator of good gut health. In particular, legumes, beans and fruit contain lots of fiber and can promote the growth of healthy .
• Fermented type of foods such as curd and yogurt contain healthy bacteria, mainly Lactobacilli, and can reduce the amount of unhealthy species of bacteria in the gut.
• It is a well-known fact that consumption of carbohydrate rich food and sugar mixed sweeteners increase blood sugar by stimulating the growth of unhealthy bacteria like in the gut microbiome. These are highly pathogenic because they produce endotoxins and endotoxins reside in the cell wall and are released when the cell dies and the cell wall disintegrates. When endotoxins are released in the blood stream can cause cell lysis which further leads to a systemic inflammatory and vasodilatory response. The most severe form of this is known as endotoxin shock, which can be rapidly fatal.
• Prebiotics food like artichokes, bananas, asparagus, oats and apples which are rich in fiber content stimulates the growth of healthy bacteria.
• Breastfeeding is very important for the development of the gut microbiome. Children who are breastfed for at least six months have more beneficial than those who are bottle-fed.
• Whole grains contain lots of fiber and beneficial carbs like beta-glucan, which are digested by gut bacteria to benefit weight, cancer risk, diabetes and other disorders.
• Vegetarian diets may help to reduce levels of disease-causing bacteria such as E. coli, as well as inflammation and cholesterol levels.
• Polyphenols are plant compounds found in red wine, green tea, dark chocolate, olive oil and whole grains. They are broken down by the microbiome to stimulate healthy bacterial growth.
• Probiotics are live bacteria that can help to restore the gut to a healthy state after dysbiosis. They do this by "reseeding" it with healthy microbes.
• Antibiotics kill many bad and good bacteria in the gut microbiome, possibly contributing to weight gain and antibiotic resistance. Thus, only take antibiotics when medically necessary.
Fecal Microbial Transplantation
Fecal microbial transplantation is an innovative microbial therapy for the treatment of those who are infected with pathogenic bacteria like Clostridium difficile colitis with the symptoms diarrhea, abdominal cramping and sometimes fever [5]. This particular infection is very much prevalent in old age group of people. Diagnosis is based on a stool DNA test that detects the organism. The antibiotic drugs used for the treatment of this infection include metronidazole, vancomycin and fidaxomycin and these drugs very often have side effects and may aggravate the heath condition of the patients (Figure 2). Moreover, the antibiotic drugs kill too many good bacteria and the infection also returns within a few days or weeks after finishing the antibiotic course. A report published during 2013 in the New England Journal of Medicine showed that fecal transplantation is more effective than oral administration of antibiotic drugs in preventing further recurrences in individuals who have already had recurrent C. difficile colitis. Johns Hopkins School of Medicine in US has developed this innovative fecal transplantation therapy and now is being used routinely for the patients suffering from pathogenic bacterial infections. Fecal transplantation is usually performed by colonoscopy and during colonoscopy therapy the colonoscope is advanced through the entire colon. As the colonoscope is withdrawn, the donor stool is delivered through the colonoscopy into the colon (Figure 3). However following precautions are taken by the doctors prior to fecal transplantation

Figure 2. Faecal microbial concentrate in syringes (source: internet web).
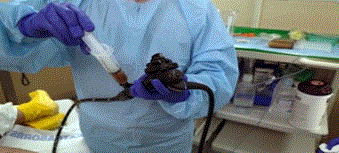
Figure 3. Faecal microbial transplantation process through colonoscopy (source: internet web).
• Patients need to stop any antibiotic therapy two days before the operation.
• It is advised to follow a liquid diet followed by an enema or laxative preparation the night before the scheduled procedure.
• Inform the doctors if the patients have any allergies.
• Patient’s medication history is most essential.
Generally the donor of the faecal microbiome transplantation has to take some precautions. Only healthy people who have no history of bowel problems and have regular bowel movements are permitted to go through the extensive screening process. It is compulsory that the donor should not have illness or the health disorders in his body. Such persons are generally identified as potential candidates and then they must complete a series of blood and stool tests for all known and detectable pathogens and diseases. Only after these three stage process have been completed and the candidate has passed all steps, then only he will be approved as a donor but screening continues on a regular basis whilst they are participating on the faecal microbial transplantation program.
About Human Microbiome Project (HMP)
Microbiome or the microbes are very important not only for the human beings but they also play pivotal role for animal and plant life as their presence in the surroundings is most essential for the survival and sustenance of entire biological forms of life [6]. Microbiome community associated with human body during birth and after that till death are involved in carrying out various physiological functions though few microbes which are pathogenic may be harmful to the body. Microbes are found in many parts of the body, like skin, gastrointestinal tract, mouth, respiratory tract, urinary tract, and vagina. The human respiratory tract, mainly nose, is colonized by Staphylococcus aureus, which is main cause of surgical wound infection [7]. The mouth contains biofilms of Streptococcus mutans, which are present as plaque on teeth surface. Similar to the skin, and unlike small intestine, not many microbes live in the stomach, because of the gastric acid, Helicobacter pylori is an example of stomach bacteria. Considering the significant role played by the microbiome community associated with different body parts the National Institutes of Health, US in the year 2007 initiated a project on Human microbiome and the focus of the project was to study the microbes which are living in and on the human body and develop a catalogue and the genetic identity of the microbiome species and characterize them. Since launch HMP in late 2007, the project received $ 153 million from Common Fund of National Institutes of Health (NIH) and $ 20 million an additional support [8]. This project was planned with different goals to achieve including investigation of microbiome community in different groups of people and on the different sites of the human body, and also their correlation with different health conditions and explain whether there are any relationships between changes in microbiome and disease. In addition, the Project has contributed in developing new fields in the technological advancement and also bioinformatics tools, through five year effort.
Though research on the microbiome is considered an emerging science, there are many research areas in this field where we to pay lot of attention and attempts have to be made in that direction. In the current scenario all over the world biomedical research work is being carried out on human microbiome and this field is progressing rapidly. Researchers are making significant headway not only understanding what the microbiome does, but how the microbiome influences human health and disease especially through its interaction with diet. Several protocols are being developed to build healthy microbiome community in the body system to create healthy environment. Evidence suggests that gut microbes and their human host share much of the same metabolic machinery. It has been also established that the diet always influences the microbiome composition, with significant implications for disease risk. This growing understanding of the role of diet in microbiome-human interactions is creating much interest and investment in developing probiotic and prebiotic food products as a means to help to build and maintain health.
Citation: Diwan A, Harke S (2021) Bank on Microbiome to keep the Body Healthy. J Nutr Food Sci. 11:791.
Received: 01-Feb-2021 Accepted: 15-Feb-2021 Published: 22-Feb-2021 , DOI: 10.35248/2155-9600.21.11.1000791
Copyright: © 2021 Diwan A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.