Journal of Clinical and Experimental Ophthalmology
Open Access
ISSN: 2155-9570
ISSN: 2155-9570
Research Article - (2011) Volume 2, Issue 5
Purpose: To evaluate the relationship between the integrity of inner segment /outer segment (is /os) junction in OCT and final VA in patients, treated for diabetic macular edema.
Methods: In this retrospective non comparative case series, 42 eyes from 33 patients with resolved diabetic macular edema were included. All of these patients had pre and post treatment Opical coherence tomography ( OCT) images and based on final status of IS/OS junction were divided into two groups. Finally visual acuity and some other clinical findings were compared between IS/OS positive and IS/OS negative patients.
Results: From these 42 patients 24 were IS/OS positive and 18 were IS/OS negative. Final visual acuity in IS/OS positive group (Log MAR 0.2667) was significantly better than IS/OS negative group ( LogMAR 0.4389 ).( P< 0.038). In this study, there was no significant difference between two groups in terms of other factors such as age, sex, duration of diabetes, type of treatment, initial VA, level of lipids, level of Hb A1c and other interfering factors.
Conclusion: There is a direct link between Status of photoreceptor layer in OCT and visual acuity, meaning that patients with DME having an intact IS/OS junction will have a better visual outcome.
Diabetic macular edema is the leading cause of visual loss in patients with non proliferative diabetic retinopathy [1]. Annually almost 75000 new cases with diabetic macular edema (DME) in the USA can be seen [2]. The ETDRS investigators defined clinically significant macular edema (CSME) and recommended laser photocoagulation for them [3]. DME is the consequence of accumulation of fluid in the retina after dysfunction of the blood retinal barrier [4]. In ETDRS, focal photocoagulation in eyes with CSME lowered the risk of moderate visual loss, increased the chance of visual gain and reduced macular thickening [5]. Other common modalities for treatment of DME are intravitreal injections of corticosteroids (triamcinolone ) and anti VEGF agents [6,7].
The conventional methods for diagnosis of DME are slit lamp biomicroscopy and fundus photography, but these are neither objective nor completely sensitive [8]. Another diagnostic modality for diagnosis of DME is fluorescein angiography that is especially valuable in assessment of vascular leakage, but its usefulness is restricted [9]. After the invention of Optical coherence tomography (OCT) images, especially SD - OCT, Ophthalmologists have been equipped with a valuable tool for diagnosis and monitoring of diabetic macular edema. OCT is used for assessment of photoreceptor layer of retina [10].
After some reports that clearly explained the relationship between the status of photoreceptor layer in OCT and visual acuity in various diseases such as BRVO [11] and CSR [12] the researchers decided to investigate this relationship in patients with DME. In present study, the researchers considered the status of photoreceptor layer of fovea after treatment of DME by photocoagulation and/or intravitreal injections and evaluated the relation between the integrity of this layer and the final visual acuity.
In this retrospective, non comparative case series, all the medical records of the patients who had been treated with laser or intra vitreal injections for DME between January 2009 and January 2010 were reviewed. The diagnosis of CSME was based on clinical examination with slit lamp and a 90 - degree lens and confirmed by OCT and FA findings. From these patients everyone who had resolved CSME was selected and enrolled in the study. The exclusion criteria were the presence of other retinal diseases, previous Panretinal photocoagulation (PRP), significant cataract that obscured fundus view for complete examination, foveal ischemia more than 2 disc diameters and visual acuity less than 20/400 before treatment.
Finally out of 52 eyes, 42 eyes from 33 patients were included in this study. For all the cases pretreatment and final best corrected visual acuity were measured with snellen chart. All visual acuity measurements were converted to Log MAR equivalents for statistical analysis. All the patients had an OCT scan of the central macula with Cirrus OCT before treatment and after completion of treatments. Then the data such as central subfield thickness (CSF), macular volume and mean macular thickness before and after treatment were considered. Two experienced observers who were masked to patients' data, evaluated the status of IS/OS line independently. These observers classified patients in two groups: 1. IS/OS positive that had completed IS/OS band 2. IS/OS negative, who had incomplete or absence of IS/OS band.
T test was applied to compare the distribution of age, sex, presence of hypertension, type of treatment, levels of triglyceride and cholesterol and also Hb A1c between the two groups and to evaluate the relation between decreased macular thickness and final visual acuity Pearson Correlation was used. Finally another t test was run to compare final VA between two groups.
42 eyes from 33 patients were included in this study. The mean age was 60.38 years. 50 percent of patients were male and 50 percent were female. The initial visual acuity (VA) means was 0.4190 Log MAR. Twenty four eyes (57.5%) were IS/OS positive and 18 (42.8%) were IS/OS negative. The initial CSF mean was 381.6 micron and macular volume mean was 11.90. At the end of the treatment CSF mean and macular volume mean were 263.4 micron and 10.65 micron respectively. Final VA means was 0.3405 Log MAR. The baseline data for demographic and clinical characteristics are presented in Table 1.
| IS/OS * Positive group | IS/OS Negative group | |
|---|---|---|
| No of eyes | 24 | 18 |
| Age (years) | 59.45 (mean) | 61.61 (mean) |
| No of women | 8/18 | 13/24 |
| Duration of diabetes (years) | 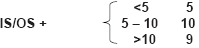 |
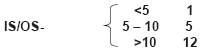 |
| Type of treatment (insulin) | 6 | 5 |
| Mean visual Auity (Log MAR) | 0.3958 (mean) | 0.4500(mean) |
| Mean Hb A1c | 7.9542 | 8.1239 |
| Mean initial CSF (micro meter) | 359.79 | 410.88 |
| Mean triglyceride level (mg/dl) | 175.75 | 162.33 |
| Mean cholesterol level (mg/dl) | 178.16 | 186.61 |
| hypertension | 14 | 7 |
Table 1: Baseline Demographics and Clinical Characteristics.
| IS/OS Positive group | IS/OS Negative group | P value | |
|---|---|---|---|
| Initial VA (Log Mar) | 0.3958 +/_ 0.3276 | 0.4500 +/_0.2526 | 0.549 |
| Final VA (log mar) | 0.2667 +/_ 0.2582 | 0.4389 +/_ 0.2546 | 0.038 |
| No of lasers | 1.125 +/_ 0.4484 | 1.00 +/_ 0.00 | 0.185 |
| No of injections | 0.625 +/_ 0.7109 | 1.50 +/_ 1.2485 | 0.06 |
| Initial CSF (micron) | 359.79 +/_ 103.60 | 410.88 +/_ 130.45 | 0.165 |
| Macular Vol (baseline) | 11.73 +/_ 1.41 | 12.12 +/_ 1.74 | 0.428 |
| Macular Vol (Final) | 10.71 +/_ 1.014 | 10.58 +/_ 1.29 | 0.719 |
| Triglyceride level (mg/dl) | 172.75 +/_ 73.57 | 162.33 +/_ 107.75 | 0.712 |
| Cholesterol level (mg/dl) | 178.16 +/_ 46.98 | 186.61 +/_ 35.79 | 0.512 |
| Hb level (mg/dl) | 13.25 +/_ 1.34 | 13.09 +/_ 1.46 | 0.716 |
| Hb A1C level (mg/dl) | 7.95 +/_ 1.56 | 8.12 +/_ 2.20 | 0.772 |
| Final CSF (micron) | 255.22 +/_ 36.44 | 269.70 +/_ 28.17 | 0.154 |
| Age | 59.45 +/_ 7.92 | 61.61 +/_ 5.52 | 0.303 |
Table 2: Final results of the study(independent t-test).
Final VA between two groups was compared. Visual acuity in IS/ OS positive group was significantly better than IS/OS negative group. (0.2667 versus 0.4389 Log MAR, P value < 0.038).
There was a negative correlation between decrease of CSF and final visual acuity. In addition the results after running t test showed there was equal distribution of basic visual acuity, basic CSF, age, sex, number of treatments, presence of hypertension, type of treatment and level of lipids and HB A1C between two groups, and none of these compounding factors were significantly different between the two groups.
Once it was a puzzlement why some patients with resolved Diabetic macular edema did not have adequate visual gain after treatment. After improvement in OCT techniques and the achievement of SD-OCT, the researchers came to more understanding about photoreceptor layer and could evaluate this layer (IS/OS junction) more easily. Recently it is emphasized that integrity of this layer is very important in visual gain in patients with resolved macular edema especially in those with BRVO or CSR [11,12]
In this study, the final status of IS/OS junction in relation with final visual acuity was considered. At the end the finding indicated that final visual acuity was significantly better in patients from IS/OS positive group. This finding is in consistent with other studies such as Sakamoto et al. who said that postoperative IS/OS junction status is related to the visual acuity after resolution of diabetic macular edema by vitrectomy [13]. In another study, Anjali S. et al. found that disruption of IS/OS junction is a very critical aspect in prediction of final visual acuity in patients with DME [14].
The present study showed that, the more decrease in CSF, the worse Final visual acuity would be. Patients with more thickened macula, before treatment would have more decline in their macular thickness; but it is clear that these patients have more problems with photoreceptor layer in advance.
The study has undoubtedly some limitations. First of all, our sample size was small and maybe with larger sample size there would be more significant difference. The second limitation might be the retrospective nature of the research and the patients did not get the same treatment.
In conclusion, this study indicated that the status of photoreceptor layer in OCT has a direct relation with visual acuity, it means that patients with DME having an intact IS/OS junction would have a better visual outcome and this can be used as a predictive factor for evaluating these cases.