Orthopedic & Muscular System: Current Research
Open Access
ISSN: 2161-0533
ISSN: 2161-0533
Research Article - (2021)Volume 10, Issue 7
Introduction: Complex tibia plateau fracture has been gradually increased, due to an increase in motor vehicle accidents. Clinical outcomes of tibia plateau fractures have been improved, due to the development of different concepts and techniques like staged surgery, combined approach, and fixation of posterior fragments. The purpose of this study was to evaluate clinical outcomes by using column-specific fixation techniques for tibia plateau fractures.
Methods: From June 2014 to May 2016, 19 cases of tibia plateau fractures were operated on in our institution. Single column fracture was fixed with a Cannulated Cancellous Screw (CCS) or single plate, two-column fractures were treated with dual plate fixation and tri-columnar fracture was fixed with three plates.
Results: The mean Rasmussen anatomic score was 16.11 (SD, 2.82; range 10 to 18). Anatomic outcome was excellent in 12 (63.3%), good in 5 (26.3%) and fair in 2 (10.5%) patients. The mean Rasmussen functional score was 26.05 (SD, 2.32; range 19 to 29). Functional outcome was excellent in 10 (52.6%), good in 8 (42.2%) and fair in 1 (5.2%) patients. Mean knee flexion at the end of treatment was 134˚ (SD, 8˚; 120˚ to 140˚), however, 3 patients had extension lag of 10˚.
Conclusion: Managing tibial plateau fracture is a challenge to an orthopedic surgeon. The column-specific fixation techniques give good anatomical reduction to restore articular congruity, rigid fixation, facilitate early motion, and better functional outcomes.
Complex tibial plateau fracture has been gradually increased, due to an increase in motor vehicle accidents [1]. The tibial plateau fracture comprises approximately 1%-2% of all fractures. It has a bimodal distribution, first occurring in young adults as a result of high-velocity injury and in the elderly as a result of a lowvelocity injury [2]. The management of these fractures remains challenging to an orthopedic surgeon. The objective of treatment is the anatomical reduction of the articular surface, soft tissue preservation, maintains the mechanical axis of the limb, rigid internal fixation to obtain a stable joint with normal functional motion [3-5].
The current treatment option includes Open Reduction and Internal Fixation (ORIF), mini-open reduction with percutaneous screw fixation and hybrid external fixation, and indirect reduction with a fine-wire circular external fixator. Every treatment has its advantages and disadvantages [6-10]. Currently, ORIF with plates and screws is considered the gold standard method of treatment. Conservative treatment is reserved for patients with undisplaced or minimally displaced fractures or minimally displaced fractures or for patients who are not fit for surgery.
Many classifications systems are available for tibial plateau fracture, among them, the commonly used are Schatzker classification and Arbeitsgemeinschaft fur Osteosynthesefragen (AO)/Orthopedic Trauma Association (OTA) classification [11- 12]. These classifications were based on the appearance of the anteroposterior radiographs. It doesn’t describe posterior shearing or coronal fractures. Luo et al introduced a CT-based three-column classification for the tibial plateau and divided the tibial plateau into three regions; lateral column, medial column, and posterior column [13]. The fractures are categorized with a single column fracture (lateral, medial, or posterior column) or different types of combined column fractures (2 and 3 columns). These days this concept has become popular in orthopedic practice. Clinical outcomes of tibial plateau fractures have been improved, due to the development of different concepts and techniques like staged surgery, combined approach, and fixation of posterior fragments.
The purpose of this study was to evaluate clinical outcomes by using column-specific fixation techniques for tibial plateau fractures.
The study was performed with the approval of our Institutional Review Board. We reviewed the medical records of 24 tibial plateau fractures from June 2014 to May 2016, at our institution. Patients of age more than 18 years with a tibial plateau fracture treated surgically were included. Patients with extra-articular fractures, pathological fractures, age <18 years, polytrauma with serious head/chest injury, Gustillo grade III open fracture, or with medically unfit for surgery were excluded. Out of 24 patients, three cases were treated nonoperatively and two cases had a vascular injury with compartment syndrome and had to refer and were excluded. Demographic data including the age of patients, gender, and mechanism of injury, closed or open fracture, and time to weight-bearing, clinical and radiological union, and complications of surgery were reviewed from patient charts.
There were 15 males and 4 females with an average age of 41.74 (Range 24 years to 78 years). The left knee was involved in 10 patients and right in 9 patients. All patients were followed till the fracture is completely united. The average follow-up is 19.5 months (range 16 months to 30 months).
The mechanism of injury was classified as
• Road traffic accidents
• Fall from a height and
• Sports-related injury The open fracture was classified according to Gustilo and Anderson classification
Plain X-rays and CT scans and 3-D reconstructions were evaluated for the size, location, and severity of articular depression and cortical split, which is useful for recognizing fragment features and pre-operative planning. The fracture was classified with Schatzker classification, AO classification, and also with a three-column concept. A three-column classification was used for decisionmaking. Use of primary treatment like bridging external fixation was also noted.
The patients were operated on using general or regional anesthesia. All patients were treated by open reduction and internal fixation with the same surgical team. The surgical approach was followed as proposed by Zhu et al. [14].
Postoperatively, a check X-ray was taken. The limbs were protected by a knee brace for 2 weeks until the subsidence of swelling and removal of stitches. Intermittent active knee mobilization was started from day 3rd onwards depending on the type of fracture, adequacy of fixation, and the treating surgeon’s judgment. The patient was discharged between 5 days-14 days after surgery, depending upon soft tissue and surgical wound condition. After two weeks, brace and suture were removed and active range of motion exercises was allowed to prevent knee stiffness and to strengthen the quadriceps.
Partial weight-bearing was allowed according to fracture healing and patient compliance. The amount of weight-bearing was selfevaluated by the patient according to the pain that it produces. Full weight-bearing was allowed after clinical and radiological evidence of healing. Weight-bearing was delayed in that patient who sustained depression fractures. Patients were reviewed at 6 weeks, 3 months, 6 months, and 1 year after the operation with a clinical and radiographic assessment of the progress of fracture healing and complications. During each visit, the patients were evaluated using the Rasmussen clinical criteria and radiological evaluation [15].
Fracture union was considered when the patient is full weightbearing without pain and the fracture site is not tender on palpation. Full weight-bearing was defined as the time that patients could have painless walking without any aids. Malunion was considered when varus-valgus angulation was more than 5˚, anterior-posterior was more than 10˚, internal and external rotations of more than 10˚, and shortening of more than 15 mm. Delayed union was defined as failure to heal after at least 4 months and no more than 9 months following surgical reduction. Non-union was defined as a failure of progressive radiographic healing over 3 months, at a minimum of 6 months from treatment [16-18].
From June 2014 to May 2016, 19 cases of tibial plateau fractures were operated on in our institution. Observation and analysis of the results were done concerning age, mode of injury, and fracture type (Table 1).
| Age in years | 24 to 78 (mean 41.74) | |||||
| Male | 15 | |||||
| Female | 4 | |||||
| Mechanism of injury | Road traffic accidents | 11 (57.8%) | ||||
| Fall | 7 (36.8%) | |||||
| sports | 1 (5.2%) | |||||
| Type of fracture | Schatzker Type | n (%) | AO | n (%) | 3 column concept | n (%) |
| I | 6 (31.5%) | B1 | 7 (36.8%) | Single Column | 12 (63.1%) | |
| II | 1 (5.2%) | B2 | 2 (10.5%) | Double Column | 6 (31.5%) | |
| III | 2 (10.5%) | B3 | 2 (10.5%) | Tri-columnar | 1 (5.2%) | |
| IV | 3 (15.7%) | C1 | 2 (10.5%) | |||
| V | 3 (15.7%) | C2 | 3 (15.7%) | |||
| VI | 3 (15.7%) | C3 | 3 (15.7%) |
Table 1: Demographic data.
The average duration of injury and surgery was 3 (range 1 to 9) days. During Surgery, column-specific fixation was done. We had 12 (63.1%) single column (medial or lateral) fractures, 6 (31.5%) two-column (medial and lateral or lateral and posterior) fractures and 1 (5.2%) tri-columnar fracture. In 3 patients (15.7%) iliac crest bone graft was used to fill the bone defect and in 4 patients (21%) local cancellous bone was elevated. In 4 patients (21%) only lag screws (cannulated cancellous screws) were used. In 15 patients (79%) locking compression plate was used. One patient had a superficial infection with implant exposed, which was resolved after debridement, implant removal (at 8 months), and IV antibiotics. One patient with open fracture (Gustillo type II) was managed with debridement and internal fixation at a single setting. Six patients had other associated fractures. Among them, two had spine fracture, one had calcaneus fracture, one had a subtrochanteric fracture, one had open tibia fracture and one had proximal humerus fracture. One patient had a sports-related injury.
With the follow-up of an average of 19.5 (range, 16 to 30) months, fracture union was observed within an average duration of 12.44 (range 10-16) weeks. There were no cases of nonunion and fixation failure. Because of implant-related local complaints, the implants were removed in 7(36.8%) patients, with a median of 1.5 years (range, 0.66 to 1.84 years).
Fifteen patients were employed at the time of injury. Eleven patients (57.8%) returned to work after a mean duration of 5.45 months (range 3 to 9 months). Four patients had to change the job due to injury.
The final assessment was done at 12 months using Rasmussen clinical criteria and radiological evaluation The mean Rasmussen anatomic score was 16.11 (SD, 2.82; range 10 to 18). Anatomic outcome was excellent in 12 (63.3%), good in 5 (26.3%) and fair in 2 (10.5%) patients. The mean Rasmussen functional score was 26.05 (SD, 2.32; range 19 to 29). Functional outcome was excellent in 10 (52.6%), good in 8 (42.2%) and fair in 1 (5.2%) patients. Mean knee flexion at the end of treatment was 134˚ (SD, 8˚; 120 to 140), however, 3 patients had extension lag of 10 degree. No patient had a fixed flexion deformity. There were no poor anatomic and functional results (Figures 1-3).
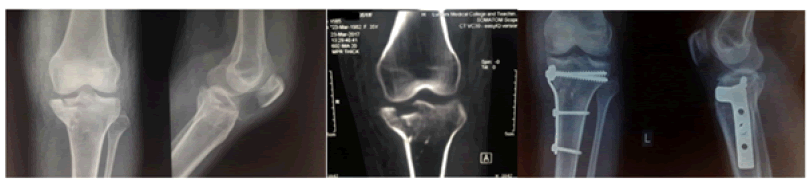
Figure 1: Medial Column fracture (single column).
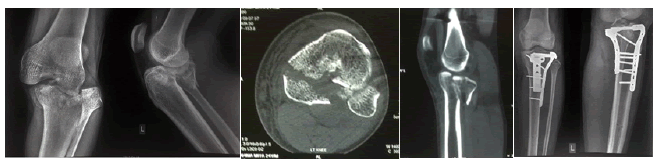
Figure 2: Two Column fracture.
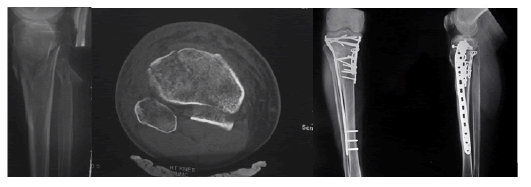
Figure 3: Three Column fracture.
Managing tibial plateau fracture is a challenge to an orthopedic surgeon. The column-specific fixation techniques provide good anatomical reduction to restore articular congruity, rigid fixation, facilitate early knee motion, and gives a better functional outcome.
The author(s) declare(s) that there is no conflict of interest regarding the publication of this paper.
Citation: Byanjankar S, Shrestha R, Sharma JR, Panthi S, Joshi RR, Dwivedi R (2021), Use of Three-column Classification System to Manage Tibial Plateau Fracture, Nepal, Orthop. Muscular Syst. 10:310.
Received: 18-Mar-2020 Accepted: 21-Mar-2020 Published: 11-Aug-2021
Copyright: © 2021, Byanjankar S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.