Journal of Clinical & Experimental Dermatology Research
Open Access
ISSN: 2155-9554
ISSN: 2155-9554
Review Article - (2019)Volume 10, Issue 3
Ultrasound elastography (USE) is an imaging technology sensitive to tissue stiffness and in recent years’ technology has enabled methods to add quantitative measurements of tissue stiffness. Most dermatologists and cosmetologists are not aware of the many useful properties of ultrasound in the clinical setting. Dermatologists interest for improved diagnostic techniques lies within the renewed medical interest in medical aesthetics application. Ultrasound can also be utilized to assess the skin’s response to treatments such as laser, mesotherapy or photodynamic therapy. Previous studies in the field of aesthetic dermatology were limited to indentometry and cutometry. Indentometry is highly subjective with low levels of accuracy and reproducibility reported from previous study findings. Cutometry is used for elasticity measures, but is not representative of the entire region of interest. Latest SWE technology provides an objective, noninvasive, whole body skin assessment. 18-22 MHz frequency probes have been shown to produce a lower signal to noise ratio, but previous studies to this extent is limited and requires further research output. Objective, non-invasive methods are there for required in practice to quantify physiological changes in the skin. Through these methods, diagnostic proficiency can be increased. The severity and progress of aging can be quantified to assess treatment outcomes.
Ultrasound elastography; Cutometry; Elastogram
Anatomy of the skin
The skin comprises of two main layers namely the dermis and epidermis.
The subcutaneous tissue is also considered a third layer of the skin due to its proximity and reactional behavior with regards to skin related pathology.
The epidermis consists of mainly keratinocytes (95%) which divides into 4 sublayers namely basal, spinous, granular and corneous layers (Figure 1).
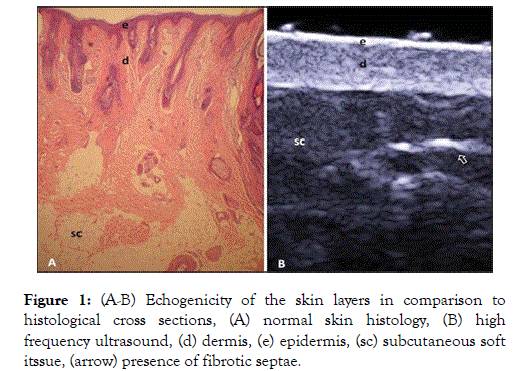
Figure 1. (A-B) Echogenicity of the skin layers in comparison to histological cross sections, (A) normal skin histology, (B) high frequency ultrasound, (d) dermis, (e) epidermis, (sc) subcutaneous soft itssue, (arrow) presence of fibrotic septae.
The excess 5% consists of fibroblasts, dendritic cells, mastocytes and macrophages.
Extracellular components include collagen and elastin fibers and amorphous fundamental substance.
The dermis is subdivided into two main compartments, the papillary and reticular dermis. The connective tissue is the most abundant component of the dermis (70%) consisting of collagen fibers.
A small interface layer is in-between the epidermis and dermis, namely a basal membrane zone, connecting the basal layer’s keratinocytes with the collagen fibers of the papillary dermis (Figure 2) [1].
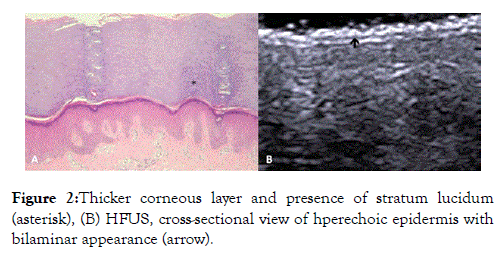
Figure 2. Thicker corneous layer and presence of stratum lucidum (asterisk), (B) HFUS, cross-sectional view of hperechoic epidermis with bilaminar appearance (arrow).
Echogenicity of the skin with ultrasound
Echogenicity refers to the level of white or black (intensity) of a structure as depicted on an ultrasound image.
Bone is a dense structure, with limited sound waves propagating through its surface during ultrasound examination, thus is depicted as black (high intensity, increased echogenicity) also known as hypoechoic.
Subcutaneous fat is of lesser density with sound waves propagating effortlessly through its layers, thus depicted as light gray (mid to low range intensity, decreased echogenicity), also known as hyperechoic or isoechoic [1,2].
The echogenicity of each layer of the skin depends on its main component:
Keratin (epidermis) - hyperechoic
Collagen (dermis) - less bright hyperechoic band
Fat lobules (subcutaneous) - hypoechoic layer with hyperechoic foci/septae within the fatty component [2].
The echogenicity and the thickness of the dermis varies with age.
In neonates, the dermis appears hypoechoic.
Patients of advanced age, or with intense actinic damage, the dermis presents with a subepidermal low echogenic band between the dermis and epidermis.
This is associated with the manifestation of elastosis and edema within the papillary dermis.
It is believed that measurement of this band could quantify actinic damage.
Ultrasound elastography
Ultrasound elastography (USE) is an imaging technology sensitive to tissue stiffness and in recent years’ technology has enabled methods to add quantitative measurements of tissue stiffness [2].
USE thus characterized the mechanical properties of biological tissues in vivo [3].
Elastography is based on the concept of changed elasticity due to changes in age and pathology, thus making it useful in diagnostic and therapeutic applications.
Conventional B (brightness) - mode ultrasound produces acoustic signals which are directed towards soft tissue structures. The reflected or back scattered tissue boundaries have distinct acoustic properties resulting in a gray scale image. USE introduces a form of mechanical excitation to deform the tissue. The tissue motion is captured by multiple B-mode images (Figure 3) [2,3].
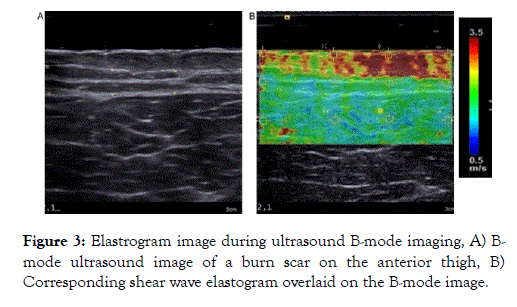
Figure 3. Elastrogram image during ultrasound B-mode imaging, A) Bmode ultrasound image of a burn scar on the anterior thigh, B) Corresponding shear wave elastogram overlaid on the B-mode image.
Previous studies have proven the applicability of elastography in various medical disciplines, primarily as a method to distinguish between normal and pathologically altered tissues.
Ultrasound elastography is used as means of novel diagnostic information for tissue disease as tissue hardness is closely related to its pathological state [4].
These studies, however, were limited to deeper anatomical structures such as internal organs, vasculature and the musculotendinous system.
The use of elastography in skin assessment can be challenging from a technical perspective. The skin is superficially located, multilayered and heterogenous in its internal architecture due to the orientation of collagen fibers. Thus elastography may be highly variable and poorly reproducible.
Such limitations have been overcome in recent years through use of high frequency ultrasound. Previous studies of the skin had sole focus on connective tissue disorders, chronic systemic inflammation and cancers. To our knowledge, limited research pertains to the analysis of normal skin and the measurements thereof by means of elastography.
By use of this ultrasound method, the biological age and parameters of skin can be analyzed as well as be used to monitor recovery of the skin after aesthetic procedures [5].
Softer tissue levels undergo more strain than a stiffer type tissue, when subjected to the same magnitude of force. Algorithms are then applied to estimate a mechanical parameter, measured as strain or elasticity, by means of an elastogram.
Each color pixel in the elastogram is an estimation of the mechanical property or parameter at that location. The elastogram is often visualized as an overlay on the B-Mode sonogram, allowing the user to interpret both structural and mechanical properties of tissue simultaneously [3].
Ultrasound has the advantage of being inexpensive, versatile and widely available.
There are two main types of elastography:
Strain imaging
Is an ultrasound technique where normal stress/pressure is applied to the tissue and the normal strain is measured (Figure 4) [2].
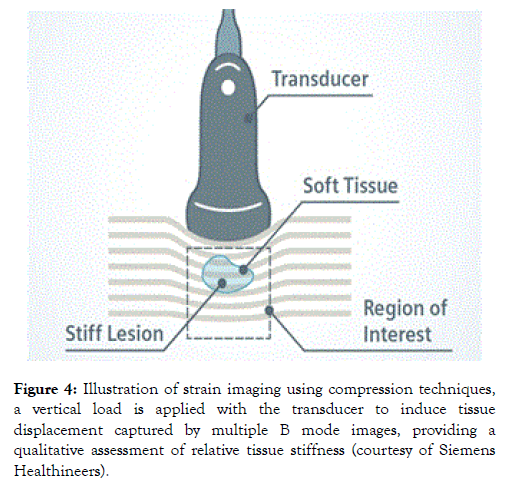
Figure 4. Illustration of strain imaging using compression techniques, a vertical load is applied with the transducer to induce tissue displacement captured by multiple B mode images, providing a qualitative assessment of relative tissue stiffness (courtesy of Siemens Healthineers).
Shear wave imaging
Is an ultrasound technique where dynamic stress is applied to tissue by use of mechanical vibrating devised in 1 Dimensional transient elastography. The shear waves created by molecular excitation during vibration, are measured perpendicular to the acoustic radiation force (Figure 5).
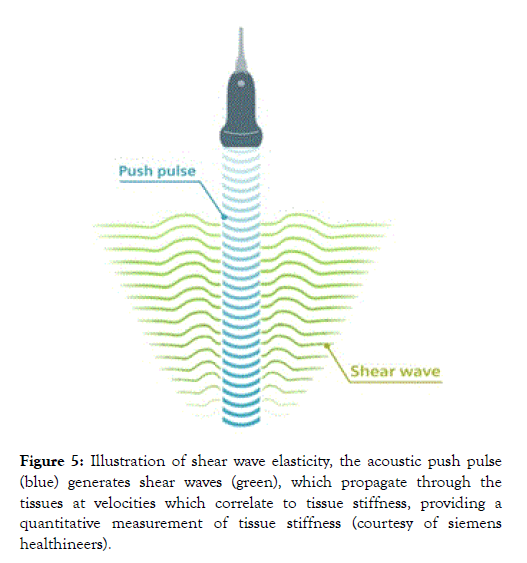
Figure 5. Illustration of shear wave elasticity, the acoustic push pulse (blue) generates shear waves (green), which propagate through the tissues at velocities which correlate to tissue stiffness, providing a quantitative measurement of tissue stiffness (courtesy of siemens healthineers).
This allows for qualitive and quantitive measurement estimates of tissue elasticity [2].
Hitachi Medical Corporation has produced echo signals captured in real-time whilst probe compression is performed through freehand compression. The strain images are then superimposed on the B-mode images with a translucent colour scale [4].
Previous studies have proven through Phantom based studies and Young’s modulus of 10kPa that small inclusions of a diameter of 2 mm can be detected in strain imaging [4].
Clinical application of elastography
Most dermatologists and cosmetologists are not aware of the many useful properties of ultrasound in the clinical setting (Figure 6) [6].
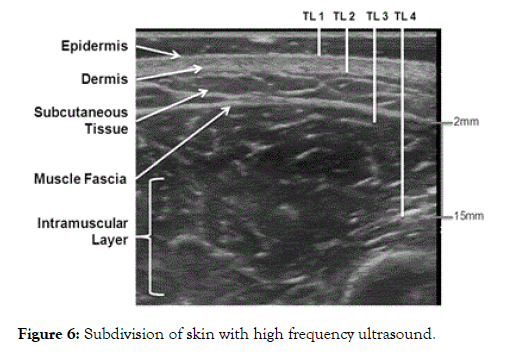
Figure 6. Subdivision of skin with high frequency ultrasound.
Regardless of the external factors affected echogenicity of the various skin layers on ultrasound, inflammatory skin diseases can be clearly defined such as:
• Visualization of subepidermal hypoechoic halo displaying a papillary dermal edema
• Local blood flow increase, as seen with Doppler/Spectral Doppler imaging.
• Homogenization of cellular tissue as seen with cellulitis.
• Detection of hyperkeratosis within the epidermis (Figure 7) [6].
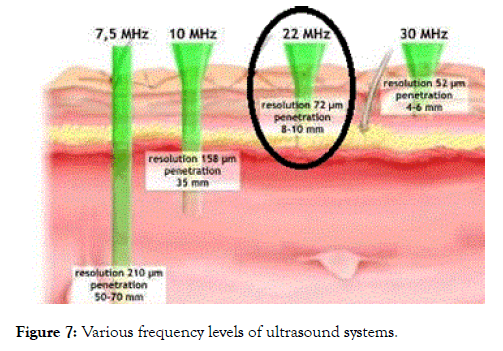
Figure 7. Various frequency levels of ultrasound systems.
These findings can assert to the best treatment methods to be used a measurable method as well to assess treatment outcomes.
Cosmetic dermatology
Dermatologists interest for improved diagnostic techniques lies within the renewed medical interest in medical aesthetics application.
Cosmetic fillers display a set of sonographic patterns that allow us to detect and identify which type of filler was used and help us in the event of complications with these agents. Skin aging assessment through subepidermal hypoechoic halo analysis is another useful ultrasound application as thickness thereof increases with photo aging (Figure 6).
Ultrasound can also be utilized to assess the skin’s response to treatments such as laser, mesotherapy or photodynamic therapy (Figure 8) [6].
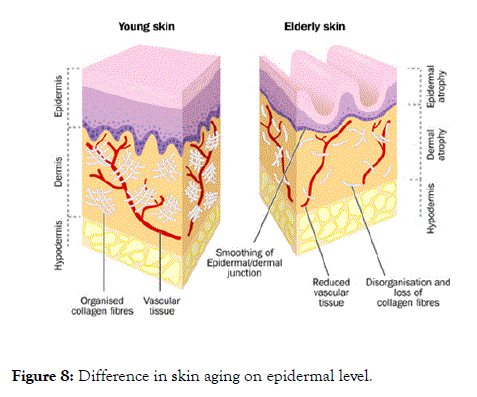
Figure 8. Difference in skin aging on epidermal level.
Limitations of elastography
Due to the increased interest of USE applications, certain technical limitations have to be addressed which could reproducibility of measurements.
Technical confounders include artifacts such as shadowing, reverberation and clutter artifacts.
Along with this, ultrasound is greatly dependent on the operator’s competency. System settings or parameters used (frequency, sampling rate, gains, etc.) can also produce biased results if not standardized across patient groups.
Thus the comparison of images from various manufacturers varies greatly.
Commercially available USE systems rely on a set of assumptions about the tissue material being assessed to simplify analysis and interpretation of images.
The main assumptions during use of USE is that the tissue is linear, elastic and isotropic (symmetrical and homogenous to stress from all directions of force).
USE also neglects to include factors such as tissue viscosity, which is directly related to shear wave frequency rates [2].
Advantages of high frequency ultrasound and shear wave technology in aesthetic medicine
High frequency ultrasound (HFUS) enables to achieve high resolution measurements with an axial resolution of 20 μm with penetration depth of 2 mm is achieved by a 75 MHz probe.
However, ultrasound units in conventional practice with a frequency of 18 MHz and higher achieves the same image quality with a large field of view during diagnostic imaging.
Previous studies have shown the use of shear wave ultrasound for the measurement of skin elasticity and the results proved a difference in the various skin layers.
Epidermis: 0.14 m/sec
Epidermal border: 0.04 m/sec
Dermis: 0.06 m/sec.
The study proved a difference in the elasticity or shear wave velocity measure between the epidermis and dermis (Figure 9) [6-10].
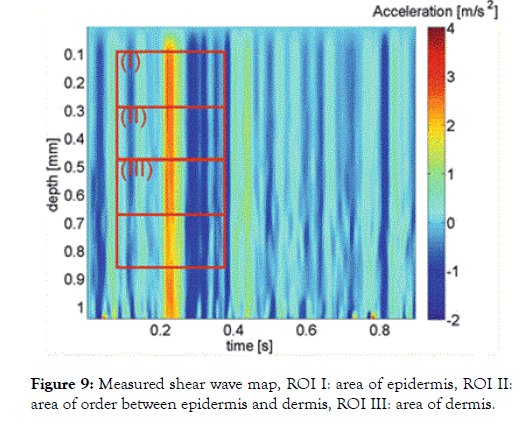
Figure 9. Measured shear wave map, ROI I: area of epidermis, ROI II:area of order between epidermis and dermis, ROI III: area of dermis.
In figure 7, a depiction of the shear wave color scale is shown for various depths of with the acceleration rate on the right, red referring to thicker/more elastic skin level and blue (-2) referring to less thick/elastic skin level.
Region of interest (ROI I) has an increased red level (4 m/sec) in comparison to ROI III (2 m/sec) dermal layers are measurable on ultrasound.
Validity and reliability of shear wave ultrasound through quantitative assessment
Skin elasticity is directly proportionate to the aging process and trauma.
Changes in the fatty and fibrous tissue parenchyma causes a change in the elastic moduli.
The physiological change which occurs during this aging process, allows for a quantifiable measurement of the skin status as seen with scleroderma or wound healing.
Thus, the solidity of skin layers can be related to the therapeutic efficacy involved during skin care treatments [3,11].
Previous studies in the field of aesthetic dermatology were limited to indentometry and cutometry.
Indentometry is highly subjective with low levels of accuracy and reproducibility reported from previous study findings.
Cutometry is used for elasticity measures, but is not representative of the entire region of interest.
Latest SWE technology provides an objective, noninvasive, whole body skin assessment. 18-22 MHz frequency probes have been shown to produce a lower signal to noise ratio, but previous studies to this extent is limited and requires further research output [11].
Objective, non-invasive methods are there for required in practice to quantify physiological changes in the skin.
Through these methods, diagnostic proficiency can be increased. The severity and progress of aging can be quantified to assess treatment outcomes [3].
Ethical approval was obtained from the Research Ethics Committee.
The study included female volunteers referred to a local aesthetic centre for use of hyaluronic fillers in the periorbital region.
Patients included in the study would be over the age of 35 years with no previous history of scarring, allergy, atopy, trauma or subcutaneous skin disorders.
All participants were subject to ultrasound evaluation by means of 18 MHz linear probe Hitachi Aloka Arietta S70 to assess the skin in the periorbital region bilaterally.
Each assessment was performed in the supine position with a gel standoff pad. The transducer was placed perpendicular to the skin. A standard image 0.5 cm lateral to the supraorbital ridge was gathered in the longitudinal plane of which various measurements were taken.
Depth to width ratio: Measurement in mm of the epidermis, dermis and subcutaneous layers (Figure 10).
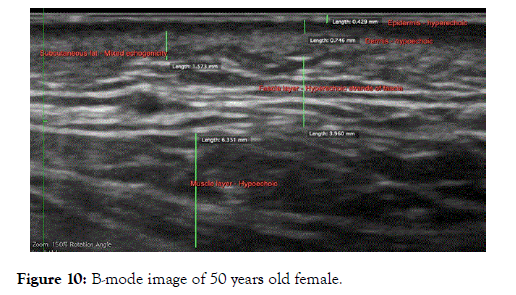
Figure 10. B-mode image of 50 years old female.
Thereafter real time elastography (RTE) was performed with biplane images of B-Mode and RTE for sake of comparison.
Various measurements were taken of the image at a standard measure of 0.6 kPa:
Fat to lesion ratio: A measurement of the epidermal/dermal skin in ovoid measure vs. subcutaneous fat tissue.
Strain ratio: A measurement of the epidermis/dermal skin layer in comparison to the subcutaneous soft tissue layer.
Histogram Tissue Width Characterization: A histogram is provided with standard mean, deviation values of the total gray scale width in selected regions namely, epidermis, dermis, subcutaneous and muscular fascia layer (Figure 11).
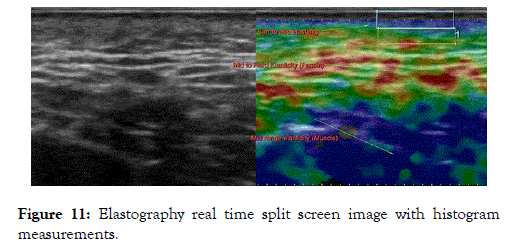
Figure 11. Elastography real time split screen image with histogram measurements.
A pilot study was performed on various female volunteers between the ages of 35- 55 years of age to assess reproducibility as well as a measurable difference between various age groups.
The results are shown below (Figures 12-14).
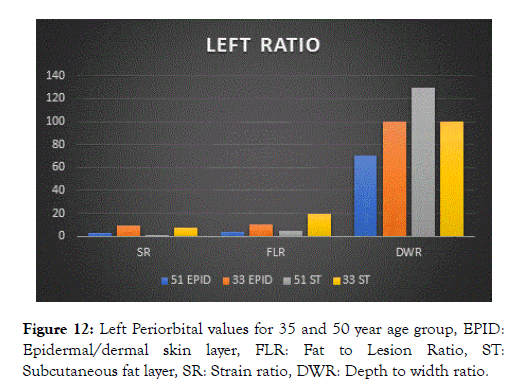
Figure 12. Left Periorbital values for 35 and 50 year age group, EPID:Epidermal/dermal skin layer, FLR: Fat to Lesion Ratio, ST:Subcutaneous fat layer, SR: Strain ratio, DWR: Depth to width ratio.
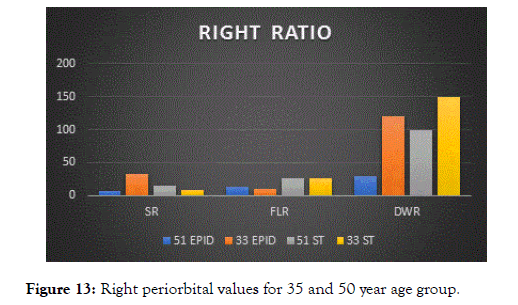
Figure 13. Right periorbital values for 35 and 50 year age group.
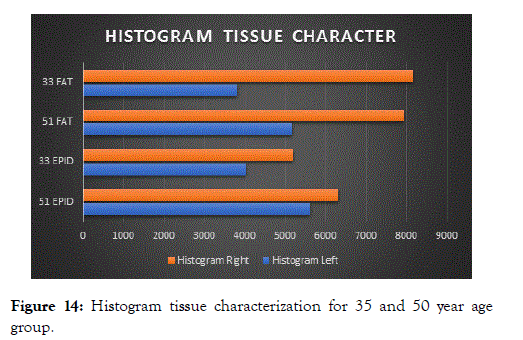
Figure 14. Histogram tissue characterization for 35 and 50 year age group.
Upon initial evaluation it is evident that the epidermal skin layer of 35 year age group has a higher strain ratio and fat to lesion ratio as the 50 year age group
The subcutaneous fat layer of 50 year age group surpasses the 35 year age group, however this is related to glabrous skin changes of aged skin.
Similar values were noted of the right periorbital region.
The Histogram Width Tissue Characterization (HWTC) between 35 and 50 year age group shows significant difference between the epidermal and subcutaneous fat tissue characterization. The epidermis layer of 50 year old female has less gray scale levels with reduced HWTC rate.
This can be prescribed to the decrease in collagen fibres, thus proving the need for treatment.
A Tsukuba Elasticity score pattern has previously been used with breast disease diagnosis, to allow a classification standard for the various color patterns noted on elastography imaging.
The color scale describes Score 1 as benign breast masses as strain seen in the entire region with color scale depicted as green (similar to surrounding breast tissue).
Score 5 is where no strain is seen within the area of interest nor in the surrounding tissue, the lesion and the surrounding tissues are depicted as blue.
Long term studies in skin elastography could promote the development of a similar classification tool for various stages of aging and the elastography measures, to determine the degree of treatment required [12].
Previous studies have demonstrated aging is associated with significant decrease in skin elasticity as proven by elastography and other measuring tools.
The above pilot study confirms these findings. A previous study assessing reference values for facial skin elasticity proved that relatively low skin thickness does note present as a confounding factor for elastography parameters.
Further studies are encouraged to include large sample populations. Following collagen filler treatment or other aesthetic methods, follow up sonography and elastography methods may prove to provide a measurable outcome in treatment.
There is limited knowledge regarding elastography, shear wave elastography and strain elastography, which provides a large field of novel research to be delved upon in future.
It is expected in future technology for tissue elasticity imaging there will be sophisticated improvements such as three dimensional and quantitative elasticity images based on elastic modulus.
Citation: Malherbe K (2019) High Frequency Ultrasound in Aesthetic Dermatology Novel Research for the use of 18 MHz Shearwave Elastography for Pre and Post Therapy Assessment: A Pilot Study. J Clin Exp Dermatol Res. 10:495. doi: 10.35248/2155-9554.10.495
Received: 07-Jan-2019 Accepted: 09-Apr-2019 Published: 16-Apr-2019 , DOI: 10.35248/2155-9554.10.495
Copyright: © 2019 Malherbe K. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.