
Journal of Clinical and Cellular Immunology
Open Access
ISSN: 2155-9899

ISSN: 2155-9899
Case Report - (2020)Volume 11, Issue 4
Introduction: Infection with tuberculosis (Mycobacterium tuberculosis) has become a disease with high incidence
and prevalence, due to its dissemination pathway and its pathophysiological mechanisms, which make it an entity
with variable clinical presentation. One of these presentations is tuberculous osteomyelitis or PottDisease. This
syndrome occurs when, by hematogenous dissemination, the mycobacterium spreads to the spinal column, most
commonly in the dorsal region, causing pain, paresis, abscesses, and deformity and, in advanced cases, paraplegia due
to neurological damage secondary to the infection.
Clinical case: In January 2018 of a male patient of 34 years old, resident of the San Quintín community, Baja
California , Mexico with type 2 diabetes mellitus, Obesity grade III, and hepatic failure as comorbidities, who
debuted with loss of mobility of lower extremities, an open magnetic resonance of the thoracolumbar spine was
performed, finding T5 body collapse plus medullary infectious process, with subsequent diagnosis bytransquirurgical
biopsy of Pott Disease , treated in the ISSSTECALI clinic, Ensenada,Baja California , Mexico during a hospitalization
period of 31 days.
Conclusion: Tuberculosis has an insidious evolution, especially when it is one of its extrapulmonary forms. Pott's
disease is one of its many manifestations, which is important to detect in the early stages to prevent complications
that compromise the patient's functionality. The treatment must be individualized according to the comorbidities of
each patient.
Tuberculosis; Pott's disease; Spine; Diabetes Mellitus; Obesity; Incidence
Tuberculosis (TB) is an infectious disease produced by microorganisms of the genus Mycobacterium, being the main etiological agent Mycobacterium tuberculosis and in more rare cases M. bovis and M. africanum. They are acid-alcohol-resistant bacilli (BAAR), strict aerobic, immobile and non-toxin-producing [1]. The pathophysiology of these microorganisms has been described through the transmission of aerosol particles that reach the alveolar space, where they are disseminated via the lymphatic system and subsequently hematogenic, thus achieving various organs. This generates a reaction of cellular hypersensitivity that favors the migration and activation of macrophages, forming a granuloma that will keep the bacillus contained in its latent state [2]. This can be reactivated during host immunosuppression states, the more severe this is, the greater degree of infection [3-6].
There are many diseases that can compromise the immune system. Adequate maintenance of the balance between immune responses and metabolism is crucial for the health-disease process, with relevant implications for disorders such as obesity, diabetes mellitus and other conditions [7]. According to the WHO World TB Report 2017, TB is the ninth leading cause of death worldwide and the first due to infectious diseases [8]. In 2016, 6.3 million new cases were reported, with the Americas contributing 222,750 cases, occupying Mexico the third place of incidence with 22,193 new cases. In Mexico, Baja California is one of the main entities in incidence and prevalence of TB, presenting a rate of 57.1, that is more than half of the new cases reported in Mexico in 2015, with a mortality rate of 7.6. [9-12]. Depending on the organ of involvement, tuberculosis can be pulmonary or extrapulmonary. Within extrapulmonary manifestations bone involvement occurs in 10% of cases, 50% of these being in the form of tuberculous osteomyelitis (Pott's disease), which affects the dorsal column, causing destruction of the vertebral bodies, being more common in underdeveloped countries and in young adults. Normally the infection starts in the anterior part of the vertebral body, spreading laterally and towards the intevertebral disc, causing compression of the spinal cord and the subsequent symptoms such as pain, stiffness, muscle spasms, abscesses and deformity, reaching in the most severe cases paraplegia [13]. The management of this pathology is complex and will depend on the clinical stage, as well as complications associated with the patient. Clinical suspicion should be made and appropriate imaging studies performed, biopsy of affected tissue with cultures and Ziehl-Neelsen staining [14].
A clinical case of a 34-year-old male patient, resident of the San Quintin delegation in Ensenada, Baja California, was presented. He had a history of admission with type 2 diabetes mellitus of one and a half years of evolution treated with metformin and obesity grade III by BMI of 42.61 kg/m2. He is referred from his locality to the Institute of Security and Social Services of Government Workers and Municipalities of the State of Baja California (ISSSTECALI) Ensenada for presenting sudden loss of strength of pelvic members of a day of sudden onset evolution accompanied by paresthesias. Associated with its symptoms is a two-week history of back pain treated with various NSAIDs, as well as epigastric pain, abdominal distension and a fever of up to 39°C. Laboratory studies at admission reported severe normocytic normochromic anemia due to Hb of 5.70 g/dL, platelet thrombocytopenia of 131,000/μL, sodium hyponatremia of 123.7 mEq/l and calcium hypocalcemia of 6.5 mEq/l. Physical examination, presented tachycardia and decreased pelvic limb strength with a score of 1/5 on the Daniels scale, still preserving sensitivity and manifesting hyperresponsiveness of osteotendinous reflexes.
During his hospitalization he presents melanogenic evacuations, so, associated with the severe anemic syndrome, three globular packages are transfused. A panendoscopy was performed, which revealed grade II/III esophageal varices and erosive gastritis with antral gastric ulcer, with mucosal sclerosis. As part of the study protocol with the suspicion of liver failure of etiology to be determined, ultrasound of the abdomen is performed, which corroborates the suspicion of portal hypertension and ascites fluid in the abdomen. During the hospital stay, the patient presents alterations in alertness, which is why management is started for hepatic enecephalopathy. Subsequently, it presents hypoesthesia in the pelvic limbs, as well as the absence of osteotendinous, cremasterian and anal sphincter reflexes. After 72 h of admission, he presents intermittent febrile peaks of predominance at night and at night, which are difficult to control. They are identified as infectious processes associated with intra-hospital urinary tract infection (UTI), which is why broad-spectrum antibiotic management is initiated.
A CT scan of the lumbar spine was performed during the 6th day of stay, with a pathological fracture of the vertebral body at T5-T6 level, confirmed by magnetic resonance (Figure 1), so that management by the neurosurgery service was initiated, requesting time for intervention. Surgical it is performed on February 12, 2018, surgical procedure consisting of T5-T6 laminectomy plus arthrodesis with transpedicular screws and T4- T6 bars as well as biopsy of associated inflammatory process, with transoperative report of vertebral tuberculosis. Treatment is started for bone tuberculosis, with rifampicin, pyrazinamide, ethambutol and isoniazid (doTBAL) (Figure 2).
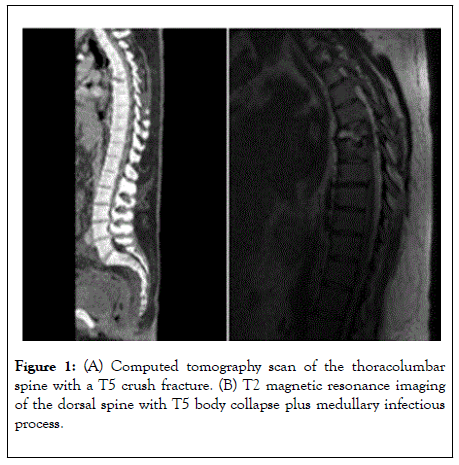
Figure 1: (A) Computed tomography scan of the thoracolumbar spine with a T5 crush fracture. (B) T2 magnetic resonance imaging of the dorsal spine with T5 body collapse plus medullary infectious process.
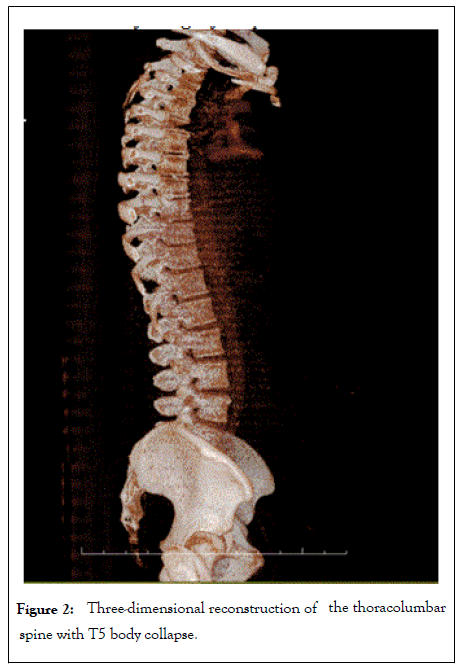
Figure 2: Three-dimensional reconstruction of the thoracolumbar spine with T5 body collapse.
During the rest of his stay, the patient presented intermittent febrile peaks with predominance of evening and night, as well as seizures managed with anticonvulsants and hallucinations managed with risperidone. He also presented an ulcer in the sacral region grade III due to prostration, which was evaluated by surgery department.
At discharge, the management of the ulcer was carried out by the unit's eschar clinic in treatment with colloid patches, it continued with data of hepatic insufficiency of unspecified etiology. A positive urine culture report was received for Stenotrophomonasmaltophilia (nosocomial acquisition) with sensitivity to levofloxacin, so it was decided to manage it as an outpatient, continuing without mobility of lower extremities and with loss of sensitivity from dermatome T9 approximately, in treatment with physical rehabilitation and with support by psychology service for being previously functional patient.
TB is pathology of great importance in our state, having a prevalence and incidence of the highest in the country and causes various complications; these are disabling and even deadly. In the case of this patient, it is known that he must have acquired the disease previously in his pulmonary form so that it could be established in the dorsal column. However, this background is not available, since both the patient and close relatives deny that he or she has been in contact with subjects with TB or that the patient has previously presented a pulmonary condition, so the chain of infection is not It has been determined.
The patient also presented with liver failure, which although could be considered as mild due to the presence of liver enzymes in the normal upper limit, complications of hepatic failure with portal hypertension and esophageal varices were evident during his study protocol. This insufficiency was invariably affected by in-hospital treatment, both anticominant and antitumor. The treatment options for tuberculsosis in this type of patient, with comorbidities such as diabetes mellitus and liver failure, is not standardized. Two of the first-line drugs that are most effective in the treatment are hepatotoxic15 and the second-line treatment is reserved for resistant mycobacteria. Therefore, the empirical onset of a treatment with second-line drugs had the possibility of generating a resistant agent, which greatly limited the therapeutic options. There were factors that delayed the management and optimal treatment due to the lack of adequate equipment to perform the corresponding image studies due to the obesity of the patient, which makes the training and equipment necessary for the management of patients with morbid obesity more and more evident. This is due to the fact that in Mexico there is still a high rate of population with overweight and obesity, having increased the combined prevalence from 71.2% in 2012 to 72.5% in 2016 [15,16].
In a review of different clinical cases presented in different countries (Spain 2001-2010, Sudan 2008-2010, Morocco 2001-2006) it can be observed that they have in common the comorbidities that our patient presents, especially DM2; The association with hepatic insufficiency was not found in any study or case report, so it would be better to explore the etiology of this condition in this particular patient. Several studies describe that Pott's disease normally occurs in children and young adults, before the third decade of life, however, in our country it has been found that the involvement between the fourth and sixth decade of life is more common. Life, as reported in this clinical case. It was also found that it affects more commonly men than women, being undoubtedly a difference diagnosis to take into account in spinal pathology in our environment [17-20].
Pott's disease is presented in an insidious and atypical way in patients in whom a thorough clinical history must be done to determine risk factors that help us to suspect this entity. It is reported in the literature that the prognosis is good for life and function while the diagnosis is made early, as well as the intervention, to avoid severe complications.
The clinical case that has been presented is an example of the diversity of presentations that have the infection by tuberculous Mycobacteria, reason why the approach and the suspicion must be carried out ideally in the first contact with the patient. Underdiagnosis of pott mal disease should be suspected in patients with risk factors (comorbidities, exposure), in endemic areas of tuberculosis, with low back pain, stiffness and muscle spasms, prior to the presence of complications such as paraplegia. Adding to the above, comorbidities such as morbid obesity and metabolic diseases in tuberculosis in a field in which more research and protocolization is still lacking. The individualization of medical treatment is, for the time being, the best management strategy, as well as the management and control of associated comorbidities. Tuberculosis is a disease that has a cure, without
However, it can be deadly and incapacitating, but it is possible to optimize time for diagnosis and timely treatment. As part of the program of the World Health Organization (WHO) "End TB" seeks to detect more cases in a timely manner and reduce the case fatality rate from 15% in 2015 to 6.5% in 2025; in Baja California the mortality rate is 7.6% in 2015, being close to international goals, however, there is a high incidence, reporting about half of new cases in Mexico, so the greatest relevance lies in the control of risk factors and transmission, in order to contribute to achieving international health goals.
Citation: González DL, Azoños CA, Sandoval RC (2020) Fracture of a Dorsal Vertebral Body as the First Manifestation of Pott's Disease. Presentation of Clinical Case. J Clin Cell Immunol.11:594. doi: 10.35248/2155-9899.20.11:594.
Received: 01-Jun-2020 Accepted: 15-Jun-2020 Published: 21-Jun-2020 , DOI: 10.35248/2155-9899.20.11.594
Copyright: © 2020 González DL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.