International Journal of Physical Medicine & Rehabilitation
Open Access
ISSN: 2329-9096
ISSN: 2329-9096
Research Article - (2020)Volume 8, Issue 5
Hemiplegic shoulder pain (HSP) is one of the most common distressing complication that patients may experience after stroke with a prevalence of 34% to 84%. Neurolysis (chemical, radiofrequency) of suprascapular nerve (SSN) is a long-lasting treatment option in treating HSP as SSN it provides 70% sensory innervation to shoulder articulation. A prospective randomized controlled trial was done to compare the effectiveness of ultrasound guided pulsed radiofrequency ablation and bupivacaine block of suprascapular nerve in reducing pain and disability in hemiplegic shoulder pain patients. Eighty-two patients enrolled in the study were allocated to 2 groups (Group A and B). Group A (n=41) received pulsed radiofrequency ablation while Group B (n=41) received bupivacaine block of SSN. Visual Analogue Scale (VAS), active and passive range of motion, SPADI were used as outcome measures. Group A showed better improvement in pain from baseline to 24 weeks as shown by reduction in VAS score from 7.11 ± 1.125 to 1.54 ± 1.02. Reduction in SPADI from 83.24 ± 9.67 to 37.02 ± 9.87 in Group A was significantly more than 84.11 ± 10.04 to 52.88 ± 12.52 in Group B (p=0.000).
Stroke; Hemiplegic shoulder pain; Radiofrequency ablation
Hemiplegic shoulder pain (HSP) is one of the most common distressing complication of hemiplegic stroke which limits range of motion (ROM), decreases hand function, delays functional recovery, extends the duration of hospitalization and can be a major factor that hinders appropriate rehabilitation. Prevalence of HSP is 34% to 84% [1,2]. Several types of pathology in HSP have been reported in the literature, and more than one type of shoulder pathology can cause pain in an individual [3]. The goals of treatment are pain reduction and improvement of ROM. As pain decreases, an exercise program can be initiated to improve ROM.
There are different methods used for alleviating pain, which includes pharmacological therapy (analgesics, anticonvulsants, steroid injection, stellate ganglion block), non-pharmacological modalities like positioning of affected limb, passive ROM exercises, sling when upright, transcutaneous electrical nerve stimulation (TENS), ultrasound therapy, functional electrical stimulation (FES) [4]. The intra-articular injection of steroids is a popular procedure, although the duration of action of such injections are limited and they are associated with several hazards and also contraindicated in diabetes mellitus patients [5].
Blocking of SSN provides significant pain relief, as it contributes 70% sensory innervation of shoulder articulation [6]. Suprascapular nerve block can be performed with local anesthetic or by electric field created by radiofrequency. There is no consensus in the literature about the ideal anesthetic drug to be used in SSNB [7]. Procedure under ultrasound guidance provides advantages like, radiation free, cost effective, safe and most importantly real time imaging.
Number of high-quality studies published on treatment of HSP are very limited. In addition, there are no studies available to compare the different treatment methods used in clinical practice directly. Therefore, the objective of the present study is to compare ultrasound guided pulsed radiofrequency ablation and bupivacaine block of suprascapular nerve in reducing pain and disability in hemiplegic shoulder pain patients. To the best of our knowledge, this is the first prospective, randomized, controlled study to investigate the effectiveness of PRF lesioning of the SSN under ultrasound guidance in patients with HSP.
A randomized control trial on 82 patients from Manipur, who were diagnosed as hemiplegic shoulder pain and admitted in Physical Medicine and Rehabilitation (PMR) ward, Regional Institute of Medical Sciences (RIMS), Imphal, India, was conducted from September 2017 to August, 2019. Approval from the research ethics board, RIMS, Imphal was taken before the start of the study and written informed consent which described in detail all aspects of the study and withdrawal process were provided to all the subjects.
Patients with HSP with pain severity with minimum score of 5 based on 10-point scale VAS (Visual Analogue Score), willingness to comply with treatment and follow-up assessments were included in the study. However, patients with mental or physical condition that would invalidate evaluation results, allergy to proposed injection agents, degenerative changes at the glenohumeral joint, any recent febrile or infectious disease (systemic and local), uncontrolled diabetes mellitus, cardiac arrhythmia or a pacemaker, hemorrhagic stroke and subjects who refuse to sign informed consent were excluded from the study.
Patients enrolled in the study were assigned into two groups (Group A and B) by block randomization method. Group A received pulsed radiofrequency ablation of the suprascapular nerve while Group B received suprascapular nerve block with bupivacaine. Both procedures were done under ultrasound guidance.
Patients were admitted in the PMR ward of RIMS, Imphal and underwent a pre-enrollment evaluation, which included demographic data, medical and surgical history with co-existing disease(s), any history of drug allergy, physical examination, baseline investigations, pain rating scores using the VAS, active and passive ROM, and Shoulder Pain And Disability Index (SPADI).
Skin over the affected side of suprascapular fossa was prepared with 10% betadine and spirit and drapes are placed over the area in a standard sterile fashion. The patients were in sitting position with the affected shoulder in full adduction and relaxed. Then ultrasound machine was positioned on the right side in front of the patient and injection site was approached from behind the patient. A thin layer of sterile gel was applied between the draped ultrasound transducer and the skin. The linear transducer was placed vertically over the fossa, first locating the scapula. After locating the supraspinatus muscle in the fossa, the probe imaged the floor or the supraspinatus fossa along its long axis. The point at which the suprascapular bone becomes discontinuous due to the suprascapular notch was identified. Bridging the notch in its base is the superior transverse scapular ligament. The SSN was found under the superior transverse scapular ligament. Overlying the ligament was the suprascapular artery, that was avoided during the needle insertion. Covering the notch were the supraspinatus and the trapezius muscle.
For pulsed radiofrequency (PRF) ablation, a 100 mm long radiofrequency needle with 10 mm active tip was advanced under ultrasound guidance toward the scapular notch after skin infiltration with 2% lignocaine. After appropriate positioning of the needle into the suprascapular notch, RF probe was inserted and checked for stimulation. Gentle adjustment of needle with sensory stimulation at 50Hz, 0.2 millisecond pulse width was used to elicit reproducible paranesthesia in the shoulder joint between 0.3-0.5volt. Motor stimulation at 2Hz frequency and 0.2 millisecond pulse width triggers contractions of the infraspinatus and supraspinatus muscles between 0.3-0.5volt. Three cycles of 120 seconds pulsed mode RF lesioning were performed keeping the temperature constant at 42 ˚ C, at a frequency of 2Hz and pulse width of 20 milliseconds (Figure 1). The 2 ml mixture of lignocaine and methylprednisolone acetate was deposited near the nerve at the end of procedure.
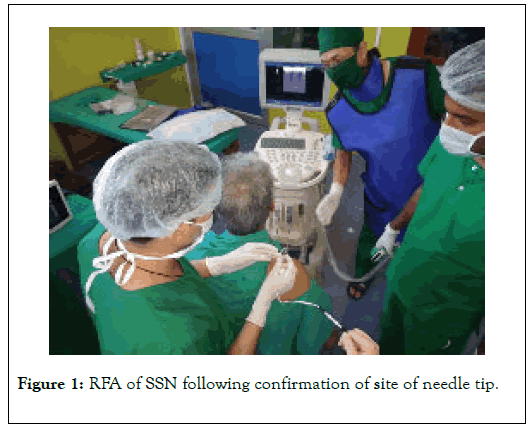
Figure 1. RFA of SSN following confirmation of site of needle tip.
For bupivacaine block, a 21-gauge needle was inserted in same manner as radiofrequency needle and 10 ml of 0.5% bupivacaine was injected. The injection and spread of local anesthetic were visualized [8].
Patients were discharged if there were no significant complications, such as pain, bleeding, or pneumothorax. Outcome variables were measured at baseline before intervention and follow up assessments were done at 1, 4, 12 and 24 weeks. VAS was used for assessing improvement in pain and active and passive ROM, SPADI were used for assessing disability during all follow up period. Patients were also assessed for intervention related adverse effects (Figure 2). Patients were asked to stop analgesics and anti-inflammatory medications if any, 48 hours prior follow up assessments.

Figure 2. Radiofrequency generator during procedure.
A sample size of 82 (41 in each group) was calculated using formulae;
n=(u+v)2× (12+22)/(1+2)2
Where, n=sample size, s=standard deviation, m=mean, u=0.84, at 80%power (1-β), v=1.96, at 5% level of significance (α) [9].
Data analysis were done using Statistical Package for Social Sciences (SPSS) version 21. Categorical variables were expressed as number of patients and percentage of patients and compared across the two groups using Chi-Square test. Continuous variables were expressed as Mean± Standard Deviation (SD) and compared across the two groups using independent t test, within the group comparison was done by paired t test. p-value <0.05 was taken as significant.
There were no significant differences in the baseline characteristics of the two groups (Table 1) and hence were comparable (p>0.05). Mean age of the patients in the Group A and Group B were 55.08 ± 5.75 and 50.89 ± 5.60 years respectively. Females constituted 25.60% (n=21) of the total patients.
| Characteristics | Group A N(SD%) | Group B N(SD%) | p-value | |
|---|---|---|---|---|
| Mean age (yrs) | 55.08 (5.75) | 50.89 (5.60) | 0.68 | |
| Gender | Male | 32 (78.05%) | 29 (70.73%) | 0.693 |
| Female | 9 (21.95%) | 12 (29.27%) | ||
| Side of affection | Right | 22 (53.7%) | 21 (51.2%) | 0.5 |
| Left | 19 (46.6%) | 20 (48.8%) | ||
| Duration (Weeks) | 17.92 (7.844) | 20.27 (8.893) | 0.951 | |
| VAS | 7.11 (1.125) | 7.05 (1.312) | 0.604 | |
| Active ROM | 33.45 (32.64) | 30.64 (29.82) | 0.394 | |
| Passive ROM | 60.64 (29.40) | 63.45 (31.65) | 0.386 | |
| SPADI | 83.24 (9.67) | 84.11 (10.04) | 0.521 | |
Table 1: Baseline characteristics of the patients.
The reduction of pain intensity was measured by VAS score showed significant reduction at the follow up periods in both the groups (Table 2). Group A showed better improvement in pain from baseline to 24 weeks as shown by reduction in VAS score from 7.11 ± 1.125 to 1.54 ± 1.02. Reduction in SPADI from 83.24 ± 9.67 to 37.02 ± 9.87 in Group A was significantly more than 84.11 ± 10.04 to 52.88 ± 12.52 in Group B (p=0.000).
| Para-meters | VAS | Active ROM | Passive ROM | SPADI | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Study group | Control group | p-value | Study group | Control group | p-value | Study group | Control group | p-value | Study group | Control group | p-value | |
| 1 week | 4.34 (1.15) | 4.20 (1.21) | 0.576 | 40.47 (34.26) | 38.69 (29.4) | 0.423 | 93.69 (22.19) | 124.15 (23.75) | 0.437 | 60.59 (12.44) | 64.51 (11.71) | 0.145 |
| 4 weeks | 2.34 (0.88) | 3.95 (1.22) | 0 | 51.57 (31.73) | 47.56 (30.03) | 0.198 | 111.26 (54.70) | 96.13 (24.56) | 0.002 | 48.37 (9.84) | 59.49 (12.43) | 0 |
| 12 weeks | 1.68 (0.90) | 3.41 (1.36) | 0 | 59.24 (32.1) | 51.05 (29.22) | 0.1 | 118.75 (8.75) | 100.75 (20.52) | 0.001 | 38.78 (9.83) | 54.46 (12.43) | 0 |
| 24 weeks | 1.54 (1.02) | 2.98 (1.37) | 0 | 60.15 (31.97) | 43.95 (29.25) | 0.038 | 119.50 (9.25) | 102.75 (20.78) | 0 | 37.02 (9.87) | 52.88 (12.52) | 0 |
Table 2: Mean improvement in the follow up periods.
Hemiplegic shoulder pain (HSP) delays functional recovery and hinders appropriate rehabilitation in a stroke patient. Pain reduction and improvement of range of motion are goals for treatment of HSP.
Blocking of the suprascapular nerve (SSN) is very effective in relieving pain and disability caused by HSP. This procedure was initially described by Wertheim and Rovenstein, in 1941 [10].
Pulsed radiofrequency (PRF) ablation of suprascapular nerve (SSN) is a safe and nondestructive method which provides long lasting pain relief and use of ultrasonography allowed for a more accurate and closer placement of the needle tip to the SSN. Recent evidence suggests that the electrical field, rather than the heat lesion, is responsible for the clinical effect of RF [11,12].
Similar to the results of Abdelshafi et al. [13] we found that this method provided long-term relief from pain as well as improvement in ROM and SPADI scores. The rapid onset of pain relief after PRF lesioning of the SSN apparently makes it easier for patients to tolerate rehabilitation therapy.
The improvement in VAS score and ROM showed a parallel pattern in follow-up in both groups. This is because as the pain improved, patients were able to achieve more ROM. In this study, significant changes in all shoulder ROMs and pain were observed in both groups. Degree of pain was significantly decreased a week after procedure and was always decreased compared to that of previous follow up visit.
Improvement in SPADI score was significant at 24 weeks when compared with baseline in both groups (p<0.05). Similarly, a prospective study done by Luleci et al. [14] showed statistical reduction in pain that lasted for up to 6 months after use of PRF lesioning of the SSN. Several other studies also reported that this procedure provided relief from pain and improved the ROM for 12 weeks to 6 months [15]. Reduction in pain by PRF up to 6 months explained by, time taken in regeneration of neuronal ion channel which are modulated by PRF generated electrical field.
Ultrasound guided suprascapular nerve block is a safe and effective treatment option for patients with hemiplegic shoulder pain. In this study we found that both pulsed radiofrequency ablation and bupivacaine block of the suprascapular nerve provided improvement in pain and disability up to 24 weeks. However, in view of the greater pain relief and disability reduction provided by pulsed radiofrequency ablation of suprascapular nerve, it is suggested that it can be the preferred treatment modality for managing pain and disability in patients with hemiplegic shoulder pain. Nevertheless, a larger sample size and longer follow up period are recommended.
Citation: Pilania C, Singh JN, Chabungbam M, Janet M, Sreejith C, Opo T, et al. (2020) Comparison of Ultrasound Guided Pulsed Radiofrequency Ablation and Bupivacaine Block of Suprascapular Nerve in Reduction of Pain and Disability in Hemiplegic Shoulder Pain: A Randomized Controlled Study. Int J Phys Med Rehabil.8:561. DOI: 10.35248/2329-9096.20.08.561.
Received: 20-Jul-2020 Accepted: 31-Jul-2020 Published: 07-Aug-2020 , DOI: 10.35248/2329-9096.20.08.561
Copyright: © 2020 Pilania C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.