Journal of Sleep Disorders & Therapy
Open Access
ISSN: 2167-0277
ISSN: 2167-0277
Research Article - (2014) Volume 3, Issue 2
Objectives: Poor subjective sleep quality in primary care has not been widely studied in Nigeria; hence this study was aimed to evaluate the subjective sleep quality and to find the association with blood pressure, depression and body mass index.
Methodology: Pittsburg Sleep Quality Index (PSQI) questionnaire was administered. Good sleep quality was defined as PSQI less than 5. The level of depression was assessed using the Patient Health Questionnaires (PHQ–9).
Results: The sample consisted of 400 subjects in the age group 18-70years. The overall mean age did 48.0 + 13.2 years, with the age group 41-50years constitute 29.5% of the studied subjects. Whilst 240 (60%) had normal blood pressure, 29(7.5%) had stage 1 and 43 (10.8%) had stage 2 hypertension. One hundred and thirty eight (34.5%) had normal weight, while 108 (27.0%) were obese. Overall sleep quality was very good, fairly good, fairly bad, and very bad in, 30.8%, 33.2%, 19.5%, and 16.5% of the respondents respectively. The prevalence of poor sleep quality was 44.0%. There was strong statistical association between poor sleep quality, blood pressure (p-value 0.002), depression (p-value 0.000) and body mass index (p-value 0.05).
Conclusion: A substantial proportion of the subjects had poor sleep quality associated with high blood pressure, increased body mass index and depression.
Keywords: Sleep quality; Hypertension; Depression; Body mass index
Sleep is a vital reparative, restorative and physiological phenomenon, and impaired sleep has significant negative impact on health [1]. The quality of sleep is a measure of both the quantitative and qualitative component of sleep. The quantitative component involves the duration of sleep whereas the qualitative components is a subjective measure of the depth and feeling of restfulness upon awakening [2]. Sleep quality is an important clinical entity for two major reasons. In the first instance, complaints about sleep quality are common; epidemiological surveys indicate that 15-35% of the adult population complain of frequent sleep quality disturbance, such as difficulty falling asleep or difficulty maintaining sleep [3]. In addition, poor sleep quality can be an important symptom of many sleep and medical disorders. One frequently measured component of sleep quality, sleep duration, may even have a direct association with mortality [4]. According to the National Sleep Foundation adults should get between 7 and 9 hours of sleep each night [5].
Sleep quality complaints are particularly relevant to physicians. Factors relating to anxiety and stress are one of the most important concomitants of sleep complaints in the general population [6]. Sleep quality represents a complex phenomenon that is difficult to define and measure objectively. It varies with sex and age. Females have higher risk of poor sleep quality [7]. Increased age is also associated with indices of poor sleep quality [8]. Bansil et al. reported that combinations of sleep disorders short sleep duration and quality of sleep were associated with increased risk in the prevalence of hypertension [9]. In another study, subjective sleep duration was negative related to depressive state [10].
The largest and longest study on adult sleep habits and weight was the Nurses’ Health Study, which followed 68,000 middle-age American women for 16 years [11]. Compared to women who slept seven hours a night, women who slept five hours or less were 15 percent more likely to become obese over the course of the study. Abdulsalam et al. [12] found no significant correlation between age, weight, height, BMI and sex of students.
Subjective Sleep quality had been associated with hypertension, depressive symptoms and higher body mass index (BMI) with paucity of data in Nigeria, hence the need for this study.
This study was conducted at the General Outpatients Clinic (GOPD) of Kwara State Specialist Hospital, Ilorin, and north Central Nigeria. The target populations were the newly registered patients attending the clinic.
The sample size was estimated using the Fisher’s Formula [13], 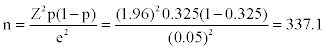 using 32.5% from a previous study [14], as the best estimate of poor sleep quality among medical students at a Nigerian University, a minimum sample size of 337.1 was calculated, but 400 was used to increase the reliability of the study.
using 32.5% from a previous study [14], as the best estimate of poor sleep quality among medical students at a Nigerian University, a minimum sample size of 337.1 was calculated, but 400 was used to increase the reliability of the study.
A systematic random sampling method was used in recruiting respondents for this study, from the period of study from October 30 to November 30, 2013. Already identified depressed subjects who were on treatment and those who refused to give consent were excluded from the study. Pretesting was carried out at the Kwara State Civil Service Hospital, using 40 respondents (10% of the sample size). Ethical approval was obtained from the Ethical Review Committee of the Kwara State Ministry of Health before the commencement of the study.
The Pittsburgh Sleep Quality Index (PSQI) was used for the subjective assessment of sleep quality [2]. The PSQI is a questionnaire consisting of 19 items which are coded on a 4-point scale (0-3) to obtain seven sub-categories, including sleep duration, sleep efficiency, sleep satisfaction, and medication use. The sum of all sub scores represents the total sleep quality score, ranging between 0-21, with higher scores representing lower sleep quality. The individuals were categorized as follows: good sleep quality (less than 5) and poor sleep quality (greater than or equal to 5). Psychometric properties have demonstrated good reliability internal consistency 0.89; test retest reliability 0.85) and good construct validity for the English language version [15].
The Patients Health Questionnaire (PHQ-9) [16] is a brief, 9 - item, patients self-report depression assessment tool that was derived from the interview-based PRIME-MD [17]. It was specifically developed for use, in primary care. It is the only tool that was specifically developed for use as a patient self-administered depression diagnostic tool, rather than as a severity or screening tool. It is the only short self-report tool that can reasonably be used both for diagnosis of DSM-4 major depression as well as for tracking of severity of major depression over time [18]. Psychometric evaluation of the PHQ-9 revealed a sensitivity ranging from 62%-92% and a specificity between 74%-88% [16-18]. All subjects screened positively for depression using Patients Health Questionnaire – 2 (PHQ-2), which was the first two questions of PHQ-9, triggered full diagnostic interviews by the behavioral scientists. Respondents who scored one and more were assessed clinically for depression. Scoring and level of depression was assessed viz: (1-4) minimal depression, (5- 9) mild depression, (10-14) moderate depression, (15-19) moderately severe depression, and (20-27) severe depression. Some direct depression care, such as care support, coordination, case management, and treatment was embarked on.
Height and weight were measured according to standardized procedures. Body Mass Index (BMI) was calculated as weight in Kg divided by height in m2 (kg/m2). The international classification of BMI was used. The principal cut-off points were as follows: moderate thinness (16.00-16.99), mild thinness (17.00-18.49), normal (18.50- 24.99), pre-obese (25.00-29.99), obese class I (30.00-34.99), obese class II (35.00-39.99), obese class III (>40.00).
An Accosson Mercury sphygmomanometer was used to measure the resting blood pressure of the subjects in a sitting position. Classification of hypertension was made according to the seventh report of the Joint National Committee on Prevention, Detection, Evaluation and Treatment of high blood pressure (JNC 7) [19] recommends the following classification of blood pressure for adults aged ≥ 18 years
Normal: Systolic: <120 mm Hg Diastolic: <80 mm Hg
Pre-hypertension: Systolic: <120-139 mm Hg Diastolic: <80-89 mm Hg
Stage 1 hypertension: Systolic: <140-159 mm Hg Diastolic: <90-99 mm Hg
Stage 2 hypertension: Systolic: ≥ 160 Hg Diastolic: ≥ 100 mm Hg
Completed questionnaire and measurements were entered into a computer data base. The data were analyzed using the epidemiological information (Epi-info) 2005 software package of Center for Disease Control and Prevention (CDC).Stepwise multiple regression analysis was conducted and poor sleep quality was significantly correlated with hypertension, depression and body mass index, the level of significance and values less than 0.05 were regarded as statistically significant.
Table 1 displays the socio-demographic characteristics of the respondents. 400 newly registered patients were recruited. Subject with the age group 41-50 constituted 29.5% of the respondents with an overall mean age of 48.0 + 13.2. Female outnumbered males. The respondents were predominantly Yoruba, 384 (96.0%) and Muslims, 354 (88.5%). Majority, 238 (59.5%) had no formal education; they were mostly traders, 156 (39.0%). Thirty (7.5%) agreed to alcohol intake. Thirty six (9.0%) formerly engaged in smoking, while 8 (2.0%) were currently smoking Table 2 shows the association between sociodemographic factors and PSQ 1 scores. Marital status (p-value .020) and ethnicity (p-value .053) were significant.
| Variable | Frequency | (%) | Mean | Std. Deviation |
|---|---|---|---|---|
| Age | 4 58 64 118 100 59 |
1.0 14.5 16.0 29.5 25.0 14.0 |
48.0 | 13.16 |
| ≤ 20 21-30 31-40 41-50 51-60 ≥ 61 |
||||
| Gender | 96 304 |
24 76 |
||
| Male Female |
||||
| Ethnicity | 8 384 6 2 |
2.0 96.0 1.5 0.5 |
||
| Hausa Yoruba Igbo Others |
||||
| Religion | 46 354 |
11.5 88.5 |
||
| Christianity Islam |
||||
| Marital Status | 250 24 14 26 82 4 |
62.5 6.0 3.5 6.5 20.5 1.0 |
||
| Married Single Divorced Separated Widow Widower |
||||
| Educational Level | 238 48 62 52 |
59.5 12.0 15.5 13.0 |
||
| Non-formal Primary Secondary Tertiary |
||||
| Occupation | 156 56 126 50 12 |
39.0 14.0 31.0 24.0 76.0 |
||
| Trader Civil Servant Self Employed Unemployed Student |
||||
| Alcohol Intake | 30 370 |
7.5 92.5 |
||
| Yes No |
||||
| Smoking Status | 356 36 8 |
89.0 9.0 2.0 |
||
| Never Former Current |
Table 1: Socio-Demographic Characteristics of The Respondents.
| Variables | PSQI SCORES | Total | p-value | |
|---|---|---|---|---|
| <=5 | >5 | |||
| Age Groups | 3 |
1 |
4 |
.775 |
| <=20 | ||||
| 21-30 | 35 | 23 | 58 | |
| 31-40 | 33 | 31 | 64 | |
| 41-50 | 62 | 56 | 118 | |
| 51-60 | 59 | 41 | 100 | |
| >=61 | 32 | 24 | 56 | |
| Total | 224 | 176 | 400 | |
| Sex | 48 |
48 |
96 |
.174 |
| Male | ||||
| Female | 176 | 128 | 304 | |
| Total | 224 | 176 | 400 | |
| Ethnicity Hausa |
3 | 5 | 8 | .053 |
| Yoruba | 220 | 164 | 384 | |
| Igbo | 1 | 5 | 6 | |
| Others | 0 | 2 | 2 | |
| Total | 224 | 176 | 400 | |
| Religion | 22 |
24 |
46 |
.235 |
| Christianity | ||||
| Islam | 202 | 152 | 354 | |
| Total | 224 | 176 | 400 | |
| Marital Status | 149 |
101 |
250 |
.020 |
| Married | ||||
| Single | 7 | 17 | 24 | |
| Divorced | 11 | 3 | 14 | |
| Separated | 11 | 15 | 26 | |
| Widow | 44 | 38 | 82 | |
| Widower | 2 | 2 | 4 | |
| Total | 224 | 176 | 400 | |
| Level of Education | 135 |
103 |
238 |
.547 |
| Non-formal | ||||
| Primary | 23 | 25 | 48 | |
| Secondary | 38 | 24 | 62 | |
| Tertiary | 28 | 24 | 52 | |
| Total | 224 | 176 | 400 | |
| Occupation | 94 |
62 |
156 |
.398 |
| Trader | ||||
| Civil Servant | 27 | 29 | 56 | |
| Self Employed | 68 | 58 | 126 | |
| Unemployed | 30 | 20 | 50 | |
| Student | 5 | 7 | 12 | |
| Total | 224 | 176 | 400 | |
Table 2: Association between Socio Demographic Factors and Psqi Scores at the Family Practice Clinic.
Table 3 shows that the overall sleep quality was very good, fairly good, fairly bad, and very bad in 30.8%, 33.2%, 19.5%, and 16.5% of the subjects respectively.
| Sleep Quality | Frequency | (%) |
|---|---|---|
| Very good Fairly good Fairly bad Very bad Total |
123 133 78 66 400 |
30.8 33.2 19.5 16.5 100 |
Table 3: Subjective Sleep Quality.
Table 4 shows the association between blood pressure, depression, body mass index and psqi among the subjects, at the family practice clinic.
| Variables | PSQI SCORES | Total | p-value | |
|---|---|---|---|---|
| <=5 | >5 | |||
| Blood Pressure Normal |
150 |
90 |
240 |
.002 |
| Pre-HTN | 46 | 42 | 88 | |
| Stage 1 | 9 | 20 | 29 | |
| Stage 2 | 19 | 24 | 43 | |
| Total | 224 | 176 | 400 | |
| Depression Minimal Depression |
212 |
129 |
341 |
.000 |
| Mild Depression | 12 | 42 | 54 | |
| Moderate Depression | 0 | 2 | 2 | |
| Severe Depression | 0 | 3 | 3 | |
| Total | 224 | 176 | 400 | |
| Body Mass Index Moderate thinness |
0 |
4 |
4 |
.045 |
| Mild thinness | 9 | 11 | 20 | |
| Normal | 84 | 54 | 138 | |
| Pre-obese | 72 | 58 | 130 | |
| Obese class 1 | 38 | 34 | 72 | |
| Obese class 2 | 15 | 5 | 20 | |
| Obese class 3 | 6 | 10 | 16 | |
| Total | 224 | 176 | 400 | |
Table 4: Association between Blood Pressure, Depression, Body Mass Index and Psqi among the Subjects, At the Family Practice Clinic.
Figure 1 evaluates the Pittsburgh Sleep Quality Index Score. Two hundred and twenty four (56%) scored ≤ 5 indicating good sleepers, while 176 (44.0%) scored >5 indicated poor sleepers.
The prevalence of poor sleep quality among the subjects was 44%. This was consistence with Suen and co-workers [20], in the US, who reported 42% and also similar to the findings of Krishna and colleagues with the prevalence of 42% [21], but higher than the CDC surveillance report of 35.3% [22] and the findings of Bawo and co-workers, at a Nigerian University with 32.5% [14], On the other hand, the result was lower than Seblewngel and colleagues [23], who found that the prevalence of poor sleep quality was 55.8%, Cheng et al. [24], who reported 54.7% and Adewole et al. while studying sleep disorders and sleep quality among adult’s patients presenting at the General Outpatients Department in ObafemiAwolowo University Teaching Hospital Complex (OAUTHC) in Nigeria, who reported prevalence of 50% [25].
The apparently high prevalence in this study may be attributed to lower health-related quality of life, low socio-economic status and concomitant poor medical conditions, and to snoring which is common among hypertensive subjects in South Western Nigeria [26]. In addition, it could also results from Obstructive sleep apnea (OSA) was high in Nigeria [27]. In this study, the overall sleep quality was very good, fairly good, fairly bad, very bad in 30.8%, 33.2%, 19.5%, and 16.5% of the subjects respectively. This result was higher than that of Vivek et al. [28], in Banasthali University Rajasthan, India, where distribution of sleep quality were excellent 20.4%, good 38.5%, satisfactory 35.8%, poor 4%, very poor, 1.3%.
Seblewengel et al. found out that approximately 25% had very good and 60% fairly good overall sleep quality [23].
Consistent with previous studies [29,30], poor sleep quality was associated with depression [31,32]. Depression was significantly associated with sleep complaints; a finding that was consistent with previous reports [33]. The relationship between depression and sleep disturbances was so strong that it was one of the diagnostic criteria of major depression [34]. High degree of depression and anxiety were found to be the influencing factors of poor sleep among Chinese adolescents [35].
There was a strong statistical association between body mass index and PSQI Score. Obese class 3 was poor sleepers. This was similar to the finding of Pearson et al. [36] who found that obese patient had difficulty with sleep. This result was consistence to the findings of Anne et al. [37]. However Abdul Salam et al. [12] found no significant correlation between age, weight, height and BMI.
Several studies had indicated that insufficient sleep, less than five or six hours were associated with weight gain [38]. The result of this study contrasted with Watson et al. [38] who found no relationship between subjective sleep quality and BMI and to Aylin et al. [30] who found no significant relationship between body measurement and PSQI scores [39]. Also, Van and Knutson [40] found no association between sleep quality and BMI.
In this study, there was statistical association between high blood pressure and PSQI (p-value = .002). Pooja et al. [9] found out that among people with both sleep disorder and short sleep, the likelihood of hypertension was slightly more than twice that for people with no sleep problems. This relationship may, in part, be the result of biologic mechanisms, suggesting that sleep deprivation may alter cortisol stress hormones and the sympathetic nervous system, resulting in elevated BP. In the sleep Heart Health Study, subjects sleeping ≤5 h/night had a higher frequency of prevalent hypertension [41] The Whitehall II [42] study also found that, women sleeping ≤ 5h/night had a higher risk of hypertension compared with those sleeping 7 h/night.
A large proportion of adults, attending the Kwara State Specialist Hospital, Ilorin Nigeria are poor sleepers with associated hypertension, depression and increased body mass index. Taking into account that poor sleep quality has major negative long term impact on health, prevention programs should be put in place.