
Advances in Pediatric Research
Open Access
ISSN: 2385-4529

ISSN: 2385-4529
Case Report - (2023)Volume 10, Issue 2
Tetanus is an infectious disease that can be avoided. The uncommon presentation of tetanus that involves the cranial nerves is cephalic tetanus. We describe a case of cephalic tetanus with unusual symptoms that was misdiagnosed by a few paediatricians and outlying institutions. This case is being presented to highlight the risk of cephalic tetanus due to Suppurative Otitis Media (SOM) as well as the rarity of cephalic tetanus due to its atypical age presentation and high mortality. All children who are eligible receive a primary immunisation against tetanus, along with a booster shot at the right time.
Cephalic tetanus; Infant; SOM; Immunisation
Tetanus is an exotoxin produced by the anaerobic bacterium Clostridium tetani that cause tonic muscle spasms as it progresses and has a high mortality rate. Tetanus is a disease that can be prevented, so vaccination is essential for defense [1-3]. The primary method of diagnosis is clinical; it may present as a widespread form with symptoms such as muscular rigidity and spasm, risus sardonicus, neck stiffness, dysphagia and trismus, or a localized form with symptoms such as muscle rigidity and spasm that are limited to the muscles supplied by the afflicted nerve [4-6].
A uncommon type of localized tetanus called cephalic or regional tetanus [7] can infrequently develop as a side effect of SOM or as a result of face trauma [8,9]. Two-thirds of people with cephalic tetanus may develop the generalized form of the illness; the mortality rate is between 15% and 20% [10].
In this case study, we wanted to assess the bilateral spasm in a male infant who was 1 month, 24 days old and had unusually early cephalic tetanus.
A male infant aged one month and 24 days who was from eastern Rajasthan was brought to our hospital's emergency room complaining of bilateral cheek hardening, feeding issues, and excessive crying over the previous 10 to 12 days. This patient was born to 26 years old gravida 1, para 1 mother with uneventful antenatal history. Patient was visited 3-4 pediatricians at nonmedical college health facilities but there was not response to treatment hence referred to higher centre. History revealed that patient had purulent discharge from both ears 3 weeks ago for 7-8 days, after that the family members noticed, he had been extremely restless for 5 days and had been excessively crying. He also presented with increased salivation, difficulty in feeding, asymmetrical facial looks. On physical examination, he was conscious and restless, his body weight was 4.37 kg and length were 55 cm. Hardness of the bilateral cheek as well as rigidity in both the jaw and neck muscles were noted (Figure 1).
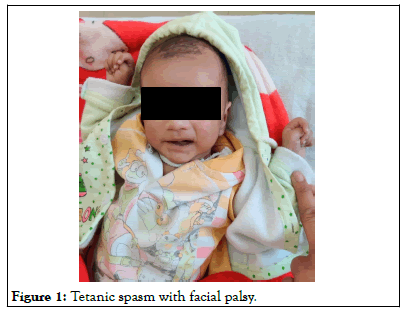
Figure 1: Tetanic spasm with facial palsy.
The baby was examined, and it was discovered that the jaw, buccal, and neck muscles had increased on-palpation tone. The skin's movement and streaking on the forehead and brows had decreased while crying. Every time the youngster grinned at her mother, this clinical symptom would appear. The outcomes of other physical examinations were normal.
The patient's consciousness was unaffected by cephalic spasm, and only the right facial nerve was paralysed during it. There was no abdominal or other muscle contraction. No active purulent discharge was present, but an otological examination revealed bilateral erythemic and inflamed tympanic membranes. The patient's complete blood count, electrolyte levels, serum calcium (total and ionic), urinalysis, and chest X-ray all fell within normal ranges, while C-Reactive Protein (CRP) was reactive and blood cultures were sterile.
The initial course of treatment included intravenous fluids and combination therapy with intravenous diazepam to control spasms. The parenteral medications were then switched over to oral form. Additionally, human tetanus immunoglobulin and the intramuscular tetanus toxoid vaccine are administered. In order to minimize extraneous stimulation (music and light), he was breastfed in a dark, quiet space. Over the course of the following week, the frequency of trismus and facial muscular spasms decreased. On the tenth day after admission, at his parents' request, he was sent home on oral valium due to domestic issues. The youngster received primary vaccination, and the parents received counseling. Subsequently presented with complete recovery of the facial nerve palsy, no spasms and minimal trismus during a follow-up visit nine days later.
One to three percent of all reported cases of tetanus are caused by cephalic tetanus, a rare form of localised tetanus characterised by trismus and paralysis of one or more cranial nerves [11]. Sometimes, as in the case of our patient, cephalic tetanus develops after SOM or craniofacial trauma [8,9]. A generalized form of tetanus with a poor prognosis develops in around two-thirds of cases of cephalic tetanus [12]. Fortunately, our patient did not develop widespread tetanus, perhaps as a result of quick treatment. This case is being discussed because localized cephalic tetanus is uncommon today and because the patient's age (1 month and 24 days) is unusual. Numerous studies have pointed to tetanus as an example of a public health system that failed because of insufficient immunization [4,13,14].
Numerous studies have clarified the role of SOM as a portal of entry in post-neonatal tetanus [4,7,13,14]. If infants exhibit facial spasms, cranial nerve palsy, and a history of SOM, we should be highly suspicious of cephalic tetanus. A successful course of treatment includes nursing care, sedation, muscle relaxation, and antibiotics. The patient fully recovered with only minor aftereffects and without developing generalised tetanus. Early detection and prompt treatment of SOM are strongly advised in order to prevent complications like cephalic tetanus. It is crucial to have both the main and booster shots as part of an appropriate preventative management plan to lower tetanus in general.
This case report highlights the rarity of cephalic tetanus, especially at an unusual age of presentation in a 1 month and 24 day-old infant. Early diagnosis and prompt treatment are crucial in preventing the progression of cephalic tetanus to the generalized form, which has a higher mortality rate. The symptoms gradually improved over the course of treatment, and the patient experienced full recovery without progressing to generalized tetanus.
This case report emphasizes the importance of primary immunization of all eligible children and booster vaccinations at appropriate times as effective strategies for tetanus prevention. Furthermore, recognizing the association between cephalic tetanus and SOM highlights the need for early diagnosis and treatment of SOM to prevent complications such as cephalic tetanus. Overall, this report serves as a reminder of the significance of vaccination programs and the importance of maintaining a high level of suspicion for cephalic tetanus, particularly in infants presenting with facial spasms, cranial nerve palsy, and a history of SOM.
The assistance of all who took part in the care of the patient is gratefully acknowledged.
CL and PJ drafted the study design, collected data, contributed in statistical analysis and inference of results. DRB AND RS supervised the entire work, drafted the study design, and collected data, contributed in statistical analysis and inference of results. DRB did critical analysis of all data, counselled the parents and hypothesized the study, drafted the study design, collected data, contributed in statistical analysis and inference of results. DRB drafted the conclusions, reviewed the literature, drafted the study design, and collected data, contributed in statistical analysis and inference of results.
This study was approved by clinical trial screening committee and ethics committee of SMS Medical College, Jaipur.
[Crossref] [Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
[Google scholar] [PubMed]
[Crossref] [Google scholar] [PubMed]
Citation: Meena CL, Jain P, Bagri DR, Sharma R (2023) Primary Immunization in Cephalic Tetanus: A Case Report. Adv Pediatr Res. 10:057.
Received: 31-May-2023, Manuscript No. LDAPR-23-23371; Editor assigned: 02-Jun-2023, Pre QC No. LDAPR-23-23371 (PQ); Reviewed: 16-Jun-2023, QC No. LDAPR-23-23371; Revised: 23-Jun-2023, Manuscript No. LDAPR-23-23371 (R); Published: 30-Jun-2023 , DOI: 10.35248/2385-4529.23.10.057
Copyright: © 2023 Meena CL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.