Emergency Medicine: Open Access
Open Access
ISSN: 2165-7548
ISSN: 2165-7548
Research Article - (2025)Volume 15, Issue 1
This study examines the awareness of occupational health hazards in prosthodontics practices among Christian dental technologists in Enugu Metropolis, Enugu state. The statement of problem is that there are numerous health related problems caused by some materials and machines used in dental prosthdontics laboratory in which prosthodontics practitioners away of in other to adopt the necessary measures to prevent the harmful effects of these materials and machineries in the human health. A descriptive cross-sectional study design was used for the study. The study for this research work was done in University of Nigeria Teaching Hospital (UNTH) Enugu, Enugu state. This research work was done in University of Nigeria Teaching Hospital (UNTH) Enugu, Enugu state. A total number of 50 Christian dental technologists were used which was gotten from the study area. The study used simple percentage, frequency and variables in analyzing one data presented by the use of tables. Findings show that based on the awareness of existence of occupational health hazards in prosthodontics practice showed that 25 (50%) strongly agree, 18 (36%) agree. According the research findings 18 (36%) agree and 24 (48%) strongly agree that provision of enough working space will help to minimize the occupational health hazards in prosthodontics practice. Recommendations were provided.
Prosthodontics practices; Christian dentist’s technologists; Health; Hazard; UNTH
Workers are central to the achievement of organizational goals and objectives. This centrally becomes threatened irrespective of worker’s knowledge, skill, experience and competence, when the workplace or the material is either unhealthy or unsafe for the worker's to discharge identified tasks. This implies that worker’s wellness and safety are critical factors to workplace performance. It is only a healthy worker that can be productive and as well, it's only a safe worker that can be comfortable at work to discharge his or her responsibilities. Workers are vulnerable to some set of hazards in their various working places known as occupational health hazards which often result to injuries, accident and a number of health Consequences. The term “hazard” refers to an inherent property of an agent or situation having the potential to cause adverse effects when organism, system or population is exposed to that agent. “Risk”, by contrast means the likelihood of causing adverse health effects. An individual’s exposure to hazard determines the degree of risk and associated untoward effects [1].
Occupational health hazard is said to be the risk to the health of a person usually arising out of employment. It’s also referring to work material, substance, process or situation that predispose or itself causes accidents or disease at workplace. Every occupation has its own health hazard which is obvious in health care system due to the nature of their jobs. Such as dental health care practitioners, physicians, nurses etc. Dental technologist which are trained and licensed dental professional who are responsible for designing, fabrication, servicing and supplying artificial appliances for a lost or congenitally missing part of the oro-facial structures as well as correction of abnormalities associated with human dentition are also victims of this hazards especially in prosthdontics practice due to the nature of their jobs and materials used in this practice.
Prosthodontics is said to be a specialty in dental technology which deals with the replacement of missing parts of teeth, bone, gums or facial structures. They are at the high risk of this occupational hazard due to the fact that this profession is practiced in the laboratory where the workers are predisposing to machines, dust particles and some of the dental materials that are in both powered and liquid forms and other agents which has the capacity to cause health related problems. According to a study conducted by Okoye, Odumegu and Omuka most workers in this profession in Nigeria were unaware of the hazardous nature of their work environment and the consequences of working in such places without adopting the relevant safety measures [2].
The statement of problem is that there are numerous health related problems caused by some materials and machines used in dental prosthdontics laboratory in which prosthodontics practitioners away of in other to adopt the necessary measures to prevent the harmful effects of these materials and machineries in the human health. This study will examine these problems. The general objective of this study is to assess the level of awareness regarding occupational health hazards in prosthdontics practice among dental technologists in Enugu metropolis, Enugu state. The specific objectives include to ascertain the social demographic characteristics of dental technologist in Enugu metropolis; to access the level of awareness of dental prosthdontics technologists in Enugu metropolis on occupational health hazards; to determine the possible causes of occupational health hazards in prosthdontics practice among dental technologists in Enugu metropolis; to evaluate the control measures taken in dental clinics to prevent occupational health hazards in prosthodontics practice among dental technologists in Enugu metropolis, Enugu state and to determine the compliance of the dental technologists to the control measures adopted in the dental clinics to prevent occupational health hazards in prosthdontics practice [3-5].
Research design
A descriptive cross-sectional study design was used for the study, to determine the awareness of occupational health hazards in prosthodontics practice among dental technologist in Enugu metropolis, Enugu state.
Study area
This research work was done in University of Nigeria Teaching Hospital (UNTH) Enugu, Enugu state. The University of Nigeria Teaching Hospital (UNTH), is a teaching hospital located in Enugu, Nigeria. It is one of the foremost and highly reputable medical schools in Nigeria. It is located along Enugu Port Harcourt express way, 21 kilometers from Enugu capital. The hospital was launched early in the 20th century as a standard healthcare center for Africans built by the colonial administrators. It later metamorphosed into a General Hospital after Nigeria gained her independence in 1960. By decree number 23 of 1974, the Federal Military Government took over the hospital, but left the management in the hands of the council of the University of Nigeria, Nsukka. UNTH Ituku- Ozalla has broad objectives of service, teaching and research. The hospital tries to achieve these through provision of inpatient and out-patient services to its clients through her highly trained staff, provision of adequate clinical materials for service and training as well as equipment for research, provision of teaching facilities for training her students and other persons in the health delivery team and conduct and promotion of research on all matters pertaining to health [6].
Study population
A total number of 50 Christian dental technologists were used which was gotten from the study area.
Sample and sampling technique
The sample sizes for the study were all the dental technologists to be drawn from the studied dental clinic within the study area. No sampling technique will be employed because the research will involve all the dental technologists available at the time of this research in the dental clinic.
Validity and reliability of the instruments
The instrument for data collection was critically reviewed by the project supervisor for necessary correction so as to ensure a valid and reliable instrument and also ensure that it covered every aspect of the research [7].
Instrument for data collection
The researcher used questionnaire in gathering data for the study. The questionnaire was defined base on the questions.
Method for data collection
The data was collected by the research student with the help of trained research assistance (supervisor) the data was collected from the selected dental clinic. The data was collected using a working questionnaire with two sections: A and B, where section A will comprises the demographic characteristics of the various respondents, while section B comprises the question relevant to the research topic [8].
Method of data analysis
The data for all analysis was generated from the questionnaire and the data collected was entered into the computer software for statistical analysis. The researcher will use simple percentage, frequency and variables in analyzing one data presented by the use of tables.
Test of hypothesis
The hypothesis was tested using Z-test, mathematically represented as follows:
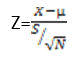
Statement of hypothesis
Ho: There is significantly adequate level of awareness regarding occupational health hazards in prosthodontics practice among dental technologists in Enugu metropolis, Enugu state.
Ha: There is no significantly adequate level of awareness regarding occupational health hazards in prosthodontics practice among dental technologists in Enugu metropolis, Enugu state.
Concept of dental technology
Dental technology is an aspect of dental health care delivery which deals with the art and science of designing, fabrication and servicing of dental oral and orol-facial tissue in order to restore pathologically or surgically lost orol-facial tissues. Dental technologists are crucial part of the dental team who use their understanding of dental material science and their skills of design and fabrication to create people’s oral facial tissues. Dental technology as a field of study comprises four major divisions but interrelated areas with the soul ultimate aim of producing prosthesis worn by dental patients. The goal is to restore the oral-facial functions of the mastication, speech and aesthetics while preventing over-eruption of the opposing teeth and the drifting of the adjacent ones [9].
Prosthodontics technology: This sub-division deals with the replacement of lost tooth/teeth using removable prosthesis such as partial denture for one missing tooth or more teeth and full dentures for one missing all of their teeth either in the upper or lower jaw or both.
Orthodontics technology: This aspect deals with the correction/straightening of malposed or crowded dentition to their normal aesthetics within the limit set by biological factors using either fixed or removable appliances.
Conservative technology: This aspect of dental technology deals with the construction of fixed appliances or prostheses for the replacement of lost tooth/teeth. Such appliances are inlays, on lays, crowns, bridges, post and jacket crowns etc.
Maxillo-facial technology: This aspect of dental technology deals with the application of thermoplastic and synthetic materials for the rehabilitation of oral-facial defects where surgical construction is not feasible or is contra indicted. Such appliances maybe artificial ear, nose, eye and eyelids, skull plates, hearing aid holder etc.
Materials used in fabrication of these prosthetics are made of a variety of materials including waxes, precious and non-precious alloys, stainless steel and metals, such as gold alloy, chromium cobalt alloy etc. Or plastic vizi, acrylic resin, a variety of porcelains and combination of two or more of these materials.
All these practices are being carried out in the various laboratories with various materials and machineries and conditions which has the capacity to induce some level of discomfort or illness to the practitioner which is termed occupational hazards. Occupational hazards are said to be the risk to person's heath usually arises from the workplace [10].
Overview of occupational hazards
The history of occupational hazards awareness can be traced back to the 18th century when Bernardino Ramazzini, who is referred to as the father of occupational medicine, recognized the role of occupation in the dynamics of health diseases. Occupational hazards have been defined as the risk to the health of a personnel usually arising out of employment. It can also refer to work, material, substance, process or situation that predisposes or itself causes accident or disease at workplace. Occupational hazards as a term signifies both long-term and short-term risks associated with the workplace environment and it is a field of study within occupational safety and public health. Short-term risks may include physical injuring, while long-term risks maybe increased risk of developing cancer or heart disease and other related ailments [11].
Bernardo published his systemic study of occupational diseases in a book entitled Demorbisartifium Diatribe in the year 1713. The book had three principles causing occupational hazards, which he recognized as follows:
• Fixed working posture
• A continuous repetitive motion
• Psychological stress
These would now be referred to as repetitive strain injuries; hence, he recognized the role of occupation in dynamics of health and diseases. Handbook of occupational hazards and control for the dental workers by Government of Alberta in year 2011 classified occupational hazards into biological, chemical, physical and psychological hazards [12].
Occupational health hazards in prosthodontics dental technology practice
Dental work set up poses many risks to its employees. New Zealand studies found over 40% of dental professionals were affected with different occupational hazards and women dentists experienced double the chances of allergy occurrence, in which prosthodontics technologists are not exceptional. Prosthodontics technology as a branch of restorative dentistry that are concerned with the restoration and maintenance of natural teeth and or the replacement of missing teeth and craniofacial tissues with artificial substitutes for either cosmetic or functionality purpose are having a lot of debates about the safety of the compositions of widely used material such as impression materials, resin-based synthetic polymers, cements, alloys, dental ceramics and machineries in the prosthodontic practice both to dental personnel and patients and appropriate safety measures for the wellbeing of the personnel. Currently, there is no substantial scientific data or robust evidence warning against the continued use of any of these materials and machineries but it is of important that the health hazards caused by these materials and machineries are well known so as to adopt the appropriate safety measures for the wellbeing of the personnel [13-15].
Classifications of hazards found in prosthodontics dental technology practice are as follows:
• Biological hazards
• Chemical hazards
• Physical hazards
• Ergonomic hazards
• Psychosocial hazards
Biological hazards
Bacterial contamination from splatter and aerosol dissemination generated by high-speed instrumentation pose a significant risk for dental personnel. Apart from contamination by microorganism, the composition of aerosol produced during the use of rotary instruments is of concern. Contaminated impression (soiled with blood, saliva and other infectious materials) are another source of infection in prosthodontics practice. When plaster or stone is poured into a contaminated impression, microorganisms from its surface spread into the cast and this infected cast is ordinary handled in the dental laboratory. The plaster dust form the infected casts gets into the respiratory tract of the laboratory personnel, settles on clothes and environmental surfaces and remains viable for a considerable time. Other possible sources of infectious contamination are the Dental Unit Waterline (DUWL), Hand pieces, saliva ejectors and suction as well as other devices attached to air and waterlines.
Chemical hazards
A variety of materials which are commonly used in dentistry such as alloys, polymer materials, acrylic resins, ceramics, cements, sealers, etchants, hypochlorite, waxes and elastomeric impression materials are generally used in clinical prosthodontics practice as well as in the laboratory. Ingredients of these materials do not pose any problem for the patients but may have deleterious effects on the dental laboratory technicians during laboratory procedures such as packing, grinding and finishing the prostheses. A study reported that 53 of 70 dental technicians were affected by pneumoconiosis, which could be caused by dust from the processing of dental materials. Pneumoconiosis is a parenchyma lung disease that arises from inhalation of (usually) inorganic dust at work. Some such dusts are biologically inert but visible on a chest X-ray or CT scan. This lung disease develops after a prolonged exposure to dust inhalation and it is very disastrous to human health. Irreversible hydrocolloid powder contains about 60% diatomaceous earth, which could be inhaled and may prove to be a health risk (carcinogenic) over a long time span.
Woody et al., monitored and characterized aerosol particles from two alginates and showed that 10%-15% of the particles pose the greatest risk. With daily utilization of irreversible hydrocolloid materials in the dental office, improper handling of these materials could be hazardous to the health of dental personnel. Even though the ceramic materials are generally inert, inhalation of its dust containing free silica in dental laboratories can lead to silicosis. Silicosis is a disabling disease caused by inhalation of crystalline silica and is mostly irreversible in nature. It is one of the oldest occupational diseases and still possesses a high morbidity and mortality rate globally. Regarding the elastomeric impression materials, it is documented that the polyether materials were found to be more toxic than polyvinyl siloxane [16].
Physical hazards
Physical hazards that are commonly encountered in prosthodontic practice include direct physical trauma, heat and fire injuries to the face, the scalp and particularly the eye. Overall, 4.5% of prosthodontists have percutaneous injuries occurred/year.
Effect on the face and finger: The grinding tools are generally of high frequency and they can cause direct injury to the face and upper extremities. The effects of vibration on the hand can also result in vibration syndrome or vibration white finger. The main effects are narrowing of arteries in fingers and hands and damage to the ends of the nerves. Early symptoms include reduced blood circulation in the fingers, reduced sensitivity of the finger to pain, touch, vibration and temperature, blanching of one or more finger tips.
Effects in the eye: The Traumatic injuries to the eye in the prosthodontics practice are more common due to the usage of high speed rotating instruments like trimming burs which can generate projectile up to 9 m/s which are often hot, sharp and infected. Symptoms includes: Lacrimation, pain, conjunctivitis, corneal abrasion and blurring of the vision. Eye irritations may happen from a variety of laboratory materials. Painful reactions are elicited when methyl methacrylate monomer or when pumice which contains lime and quartz are accidentally splashed into the eye; in addition, pumice can also cause eye abrasion.
Curing lights are commonly used for polymerization of restoration resin materials. They emit intense blue light in the range 400 nm to 500 nm wavelength. According to a report, the increased ocular risk occurred at about 440 nm. That's to say, high irradiance of blue light can be toxic to test animal’s cellular structures and human fetal retinas. When the blue light strikes the retina, they inhibit the formation of cytochrome-c-oxidase, which transports oxygen to photoreceptors and other retina calls which leads to degeneration of retina [17].
Effect in the ear: Noise levels at a given intensity and duration in any environmental situation is a potential health hazard. Loss of hearing and tinnitus are the common side effects of noise beyond the permissible level in a set up.
According to Occupational Safety and Health Agency (OSHA), Exposure to 85 dB of noise, known as an exposure action value, for more than eight hours per day, can result in permanent hearing loss.
Ergonomic hazards
Ergonomic hazard is a physical factor within the environment that harms the musculoskeletal system. Dental professionals are notably affected with musculoskeletal diseases in their career. The potential manifestations include various Musculoskeletal Disorders (MSD) that are characterized by the presence of discomfort, disability or persistent pain in the joints, muscles, tendons and other soft parts. The risk factors comprise repeated movements and prolonged awkward or forced body postures. According to a prevalent study, 62% of dentists reported at least one musculoskeletal compliant, 30% showed chronic complaints, 16% had spells of absence and 32% sought medical care.
Prosthodontists are at high risk of neck and back problems due to the limited work area and impaired vision associated with the oral cavity. These working restrictions frequently cause them to assume stressful body positions to achieve good access and visibility inside the oral cavity which result in awkward positions over long periods of time; which in turn result in back problems. The symptoms include low back pain, stiffness and sciatica with neurological features such as tingling, paresthesia and muscle weakness. An electromyography study identified that shoulder, neck and arm muscle were placed under the most stress by routine dental work.
In another study, the Nebraskan dentists reported that crown and bridge work was most likely to evoke altered sensations in their upper limbs. Tendinopathies and carpal tunnel syndrome were associated with both repetitive work and forceful work. The hand performs many complex tasks and the tendons move inside tendon sheaths with synovial fluid. Repetitive and forceful movements and the use of vibrating tools increase fluid accumulation and inflammation. Symptoms can appear from any activity causing prolonged increase in passive or active pressure in the carpal canal. According to Fish and Morris percentage of carpal tunnel syndrome subjects in the general population were work-related and often associated with repetitive motions.
Psychosocial hazards
These physical and emotional demands may result in physical and mental burnout. Occupational stress such as coping with difficult or uncooperative patients, over workload, constant drive for technical perfection, dissatisfaction in treatment is common among dentists. The most common factors contributing to stress at work were patient demands (75%), practice management/staff issues (56%), fear of complaints/ litigation (54%) and non-clinical paperwork (54%).
These physical and emotional demands result in physical and mental burnout. A comparison of stress levels and coping stress in male and female technicians showed that stress levels were similar, although women experienced more personal and domestic stress. Regarding coping response, both sexes exhibited similarity in most respects, except that women were more inclined to discuss their problems [18].
Risk factors associated with occupational health hazard in prosthodontics practice
Dental personnel are exposed to various occupational health hazards like stress, allergic reactions, higher noise levels, accidental splashing of irritant materials, radiation, musculoskeletal disorder etc. Dental prosthodontics are also associated with significant risk of exposure to various microorganisms in infectious agent which may be present in blood or saliva normally found on impression, as a consequence of bacteremia or viremia associated with systemic infection dental health care worker may be exposed to variety of micro-organisms via blood or saliva. The national institute for occupational safety and hazards, list the following workplace factors that can result to hazards.
• Job task demands (work overload, lack of task control, role ambiguity).
• Organizational factor (poor interpersonal relations, unfair management practice).
• Financial and economic factors.
• Inadequate staffing level.
• Exposure to infectious and hazardous substances.
• Poor ventilation.
• Ignorance.
• Negligence.
• Wrong use of instruments.
• Wrong working posture.
• Poor method of sterilization.
Management of occupational health hazards
U.S public health service explained the various methods of management of health hazards to be:
Identification: This is the process of identifying all new and existing hazards that occurs in the dental clinic.
Elimination: This is proper disposal of material that could cause or result to hazards proper/appropriate medical history/medical record taking and frequent review or update
Substitution: Substituting hazards may not eliminate all hazards but may lessen the harm or danger that the hazard poses. Substitution can only be done when the hazards cannot be eliminated.
Isolation: If the hazards cannot be substituted, isolation of materials or equipment’s can be done to achieve safety (freedom from hazards).
Prevention and control of occupational health hazards in prosthodontics practice
The basic goal of Occupational Safety and Health Agency (OSHA) is to educate employers and employees about the work place hazards, risk assessment and risk management strategies. The degree of risk might depend on several factors including age, personal susceptibility, total daily exposure, exposure measured over the years and medication. It is the responsibility of professionals and technicians to understand the specific risk factors or hazard agents and formulate an effective preventive management protocol.
Modern prosthodontics practice is equipped with sophisticated work area designs with adequate ventilation and advanced armamentarium that could possibly reduce noise pollution and risks associated with chemical and ergonomic hazards. Use of masks and aspirators and mechanical removal of as much resin as possible before using rotary instruments may reduce the biological exposures. An orange shield used with the curing equipment adequately filters blue light between 350 nm to 500 nm. Apart from this, blue light filtering spectacle with side shields help to protect against reflectance and scatter [19].
Control measures for physical hazards
Use of face shield or shatter resistant eyeglasses with side shields, ear plugs, splash guard’s/safety guards for lathes and table top rotary devices, fire extinguishers.
Control measures for chemical hazards
• Use of local exhaust ventilation systems.
• Adequate fume extraction system, aerosol/dust evacuation hood in the dental laboratory.
• Appropriate use of personal protective equipment’s. vinyl gloves.
Control measures for biological hazards
OSHA guideline exposure control plan, exposure control precautions, laundry procedures, housekeeping standards and waste disposal regulations.
Control measures for ergonomic hazards
• The practitioner should take at least 6 minutes of rest every hour.
• Proper ergonomic dental unity design.
• Personalized rehabilitation exercises, stretching and regular aerobic activity.
• Avoid prolonged extension, bending or twisting of the wrist and keep head fairly straight and elbow close to sides.
Control measures for psychosocial hazards
Stress management workshops, deep breathing exercises, relaxation, hypnosis and desensitization technique.
Substitution: Substituting hazards may not eliminate all hazards but may lessen the harm or danger that the hazard poses. Substitution can only be done when the hazards cannot be eliminated.
Isolation: If the hazards cannot be substituted, isolation of materials or equipment’s can be done to achieve safety (Freedom from hazards).
Table 1 shows that males are 19 (38%) of the respondents and females are 31 (62%) of the respondents, the age range shows that 21-30 are 31 (62%), 31-30 are 15 (30%), 41-50 is 0, 50 and above are 4 (8%). Marital status shows that single is 38 (76%), married are 12 (24%), while none of them is neither divorced nor widowed. Educational qualifications show that 33 (66%), MSc are 4 (8%), nobody has PhD years of experience shows that 35 (70%) had 1-5 years’ experience, 8 (16%) had 6-10 years’ experience, 7 (14%) had 11-15 years’ experience.
| Variable | Variable category | Frequency | percentage |
| Sex | Male | 31 | 62 |
| Female | 19 | 38 | |
| Total | 50 | 100 | |
| Age | 21-30 | 31 | 62 |
| 31-40 | 15 | 30 | |
| 41-50 | 4 | 8 | |
| 50 and above | 0 | 0 | |
| Total | 50 | 100 | |
| Marital status | Single | 38 | 76 |
| Married | 12 | 24 | |
| Divorced | 0 | 0 | |
| Widowed | 0 | 0 | |
| Total | 50 | 100 | |
| Educational qualification | HND | 33 | 66 |
| B. Tech | 13 | 26 | |
| MSc | 4 | 8 | |
| PhD | 0 | 0 | |
| Total | 50 | 100 | |
| Years of experience | 1-5 | 35 | 70 |
| 6-10 | 8 | 16 | |
| 11-15 | 7 | 14 | |
| 16-20 | 0 | 0 | |
| 21 and above | 0 | 0 | |
| Total | 50 | 100 |
Table 1: Socio-demographic characteristics (n=50).
Awareness of occupational health hazards in prosthodontics practice
Table 2 shows that 25 (50%) of the respondents strongly agrees that there are health hazards in prosthodontics practice, 18 (36%) of the respondents agree, those that strongly disagree are 2 (4%). Source of information shows that 25 (50%) of the respondents got their information through seminar, 13 (26%) got theirs through workshop, 7 (14%), through experience, 0 through TV, 5 (10%) through newspaper and 0 got theirs through radio.
| Variable category | Variable | frequency | Percentage (100%) |
| Occupational health hazards exist in prothodontics practice | SA | 25 | 50 |
| A | 18 | 36 | |
| SD | 2 | 4 | |
| D | 5 | 10 | |
| Total | 50 | 100 | |
| Source of information | Seminar | 25 | 50 |
| Workshop | 13 | 26 | |
| Experience | 7 | 14 | |
| TV | 0 | 0 | |
| Newspaper | 5 | 10 | |
| Radio | 0 | 0 | |
| Total | 50 | 100 |
Table 2: Awareness of occupational health hazards in prosthodontics practice among dental technologist.
Table 3 shows that 16 (32%) of the respondents strongly agree that inhalation of refractory materials in investment materials causes pneumoconiosis, 21 (42%) of the respondents agree, 5 (10%) strongly agree, those that disagree are 8 (16%). Inhalation of dust containing free silica causes silicosis, according to the respondents 17 (34%) strongly agree, 20 (40%) said they agree,3 (6%) of them strongly disagree while those that agree are 8 (16%). In responses to the whether constant use of vibrating tools causes vibration syndrome, 30 (60%) of the respondents strongly agree, 15 (30%) agree, 2 (4%) of them strongly disagree while 3 (6%) said they agree. On awareness of whether exposition to noise of different sound levels causes hearing loss, 23 (46%) strongly agree, 18 (20%) said they agree, those that strongly disagree are 3 (6%) while 6 (12%) disagree. don’t know. On the accidental splashing of methyl methacrylate monomer, 21 (42) of the respondents strongly agree that it causes irritation in the eye, 20 (40%) of the respondents agree, those that strongly disagree are 2 (4%), while 5 (10%) disagree.
| Variable category | Variable | Frequency | Percentage (100%) |
| Inhalation of refractory materials in investment materials causes pneumoconiosis | SA | 16 | 32 |
| A | 21 | 42 | |
| SD | 5 | 10 | |
| D | 8 | 16 | |
| Total | 50 | 100 | |
| Inhalation of dust containing free silica causes silicosis | SA | 17 | 34 |
| A | 20 | 40 | |
| SD | 3 | 6 | |
| D | 10 | 20 | |
| Total | 50 | 100 | |
| Constant use of high vibrating tool/machineries causes vibration syndrome, narrowing of arteries in the finger and hands | SA | 30 | 60 |
| A | 15 | 30 | |
| SD | 2 | 4 | |
| D | 3 | 6 | |
| Total | 50 | 100 | |
| Experience to noise of different sound levels in the laboratories causes hearing loss | SA | 23 | 46 |
| A | 18 | 36 | |
| SD | 3 | 6 | |
| D | 6 | 12 | |
| Total | 50 | 100 | |
| Accidental splashing of methyl methacrylate monomer or pumice causes eye irritation | SA | 21 | 42 |
| A | 20 | 40 | |
| SD | 4 | 8 | |
| S | 5 | 10 | |
| Total | 50 | 100 |
Table 3: Awareness of the possible causes of occupational health hazards in prosthodontic practice.
Table 4 shows that 26 (52%) of the respondents strongly agree, that provision face mask is one of the control measures of occupational health hazards,19 (38%) agree, those that strongly disagree are 2 (4%) while 3 (6%) of the respondents disagree. Awareness mechanical removal of resin in rotary instruments before use shows that 15 (30%) of the respondents, strongly agree, 26 (52%) of the respondents, agree, those that strongly disagree are 2 (4%), 6 (12%) of the respondents disagree. Provision of ventilation in the work place, the research shows that 22 (44%) of the respondents strongly it is one of the control measures for occupational hazards, 20 (40) agree, those that strongly disagree are 2 (4%) of the respondents while 6 (12%) disagree.
| Variable category | Variable | Frequency | Percentage (100) |
| Face mask provision is one of the control measures for prevention of occupational health hazards | SA | 26 | 52 |
| A | 19 | 38 | |
| SD | 2 | 4 | |
| D | 3 | 6 | |
| Total | 50 | 100 | |
| Provision of adequate working space is very important to reduce occupational health hazards | SA | 15 | 30 |
| A | 26 | 52 | |
| SD | 2 | 4 | |
| D | 7 | 14 | |
| Total | 50 | 100 | |
| Provision of ventilation in the work place is one of the control measures of occupational health hazards | SA | 22 | 44 |
| A | 20 | 40 | |
| SD | 2 | 4 | |
| D | 6 | 12 | |
| Total | 50 | 100 |
Table 4: Evaluating the control measures taken in the dental clinic to prevent occupational health hazards in prosthodontics practice.
Table 5 below shows that 25 (50%) of the respondents strongly agree that it is good to protective clothing while trimming, 21 (42%) of the respondents agree, only 1 (2%) that strongly disagree, while 2 (4%) of the respondents disagree. Responds on wearing of face mask while trimming shows that 23 (46%) strongly agree, 21 (42%) agree, those that strongly disagree are 2 (4%) while 4 (8%) of the respondents disagree. Responds on putting on face mask while handling porcelain shows that 19 (38%) strongly agree, 24 (48%) of the respondents agree, those that said strongly disagree are 3(6%), while 4 (8%) agree. Responds on having enough working space in the laboratory shows that 18 (36%) strongly agree, 24 (48%) of the respondents agree. those that strongly disagree are 5 (10%) while 3 (6%) agree. Working in a well ventilated laboratory shows 21 (42%) strongly agree that it is always very good to work in well ventilated work place, 19 (38%) agree, those that strongly disagree are 3 (6%) while 7 (14%) disagree.
|
Variable category |
variable |
Frequency |
Percentage (100%) |
|
It is good to wear protective clothing while trimming |
SA |
25 |
50 |
|
A |
22 |
44 |
|
|
SD |
1 |
1 |
|
|
D |
2 |
4 |
|
|
Total |
50 |
100 |
|
|
Wearing face mask while investing is very important |
SA |
23 |
46 |
|
A |
21 |
42 |
|
|
SD |
2 |
4 |
|
|
S |
4 |
8 |
|
|
Total |
50 |
100 |
|
|
Putting on face mask while handling porcelain is very essential |
SA |
19 |
38 |
|
A |
24 |
48 |
|
|
SD |
3 |
6 |
|
|
D |
4 |
8 |
|
|
Total |
50 |
100 |
|
|
Having enough working space in laboratory is very paramount for controlling occupational health hazards |
SA |
18 |
36 |
|
A |
24 |
48 |
|
|
SD |
5 |
10 |
|
|
D |
3 |
6 |
|
|
Total |
50 |
100 |
|
|
It is always very good to work in well ventilated work place |
SA |
21 |
42 |
|
A |
19 |
38 |
|
|
SD |
3 |
6 |
|
|
D |
7 |
14 |
|
|
Total |
50 |
100 |
Table 5: To access the compliance of the dental technologist to the measures provided in the clinic to prevent occupational health hazards in prosthodontics practice.
This research was carried out for the purpose of knowing the level of awareness of occupational health hazards in prosthodontics practice among dental technologist in Enugu metropolis, Enugu state. It was carried out in university of Nigeria Teaching Hospital (UNTH) Enugu, Enugu state.
A total of 50 dental technologists were used for the study, there were 19 (38%) males and 31 (62%) females which showed higher number of females than males. On the age range of the respondents and years of working experience, highest number of the respondents 31 (62%) were within the range of 21-30 years, 15 (30%)were within the age range of 31-40 years and the least were 4 (8%) are within the age of 50 and above. According to years of working experience, 35 (70%) has 1-5 years of working experience, 8 (16%) has 6-10 years of working experience and 7 (14%) has 11-15 years of working experience [20].
Based on the awareness of existence of occupational health hazards in prosthodontics practice showed that 25 (50%) strongly agree, 18 (36%) agree. In responds to health effects of inhalation of dust particles in the workplace, accidental splashing of methymethacrylate in the eye and effect on the working posture showed 20 (40%) agree, 17 (34%) strongly agree that inhalation of dust particles from workplace causes diverse health challenges. 21 (41%) strongly agree, 20 (40%) agree that accidental splashing of methymethacrylate monomer cause eye irritation. These finding are in consistent with A New Zealand study which found out that over 40% of dental professional’s prosthodontics practice has eyes, respiratory and systemic complains, 13% with musculoskeletal problem at some point in their career.
According the research findings 18 (36%) agree and 24 (48%) strongly agree that provision of enough working space will help to minimize the occupational health hazards in prosthodontics practice. This is in line with a research carried out in USA, Canada and UK shows that (36.4%) of the participants reported that they have confined space to work in the dental laboratories. This confinement of space alone can lead to many physical as well as psychological hazards including miss-handling of hazardous materials and technical exposure to harmful chemicals and infected human tissues.
Several occupational hazards and risks remain a serious concern in a prothodontics practice, particularly Muscoskeletal Diode (MSD), Contact dermatitis, lung diseases caused by inhalation of dust particles. Understanding the various risks will educate the professionals for a better work practice and care of personal health. A mere knowledge of such hazards and familiarity with its characteristics is not sufficient for an individual to assess the potential threat. An understanding of the extent of exposure to the hazards and strategies for minimizing the effect of occupational hazards should be followed for a safe and healthy practice.
Based on the findings of this study it is recommended that work place environment should be improved in terms of providing safety precaution measures to dental technicians. They should be instructed that all the work related health problems among them can be avoided if they use safety measures in the dental laboratories. All the personal protective measures must be available for the practitioners. Attention should be given to reduce stress by improving their salaries to deal financial stress and by giving sufficient working time to avoid work load on them. They should be trained for communication skills to develop interpersonal skills in dealing with patients. Secondly, a strict time plan and work load was found to be major stressors. The condition of some of the equipment’s in the clinic was reported to be fairly good. However, presence of safety precautions like fire extinguishers and emergency exit signs should be put in place in the dental laboratories. This will help reduce the threatening risks faced by all the dental practitioners in the dental laboratories.
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
[Crossref] [Google Scholar] [PubMed]
Citation: Uroko FC, Ogechi NF (2025) Awareness of Occupational Health Hazards in Prosthodontics Practices among Christian Dental Technologists in Enugu Metropolis, Nigeria. Emergency Med. 15:337.
Received: 01-Oct-2024, Manuscript No. EGM-24-34415; Editor assigned: 04-Oct-2024, Pre QC No. EGM-24-34415 (PQ); Reviewed: 18-Oct-2024, QC No. EGM-24-34415; Revised: 03-Jan-2025, Manuscript No. EGM-24-34415 (R); Published: 10-Jan-2025 , DOI: 10.35248/2165-7548.25.15.337
Copyright: © 2025 Luo Q, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution and reproduction in any medium, provided the original author and source are credited.