Review Article - (2020) Volume 8, Issue 2
The current level of "discussion" on these diets by many people reminds me of elementary school children fighting on the playground during recess. Ms. Michaels efforts to bring some intelligence to this discussion is different.
Despite the constant arguments about, you cannot honestly call any of this a debate or intelligent discussion, between the low carbohydrate diets and the other types of diets proposed by the diet pundits, there is little if any new or useful information. Study after study show if you change the way a person eats, they can lose weight; big deal! These same studies use changes in blood tests to support the benefit they have for reducing heart disease. These studies exclude people whose cholesterol and other blood tests for inflammation go up, thereby making the results look better, while criticizing other studies for not agreeing with them.
The major problem with this approach is that I never said that reducing your cholesterol level or your insulin resistance or your CRP level would reduce your heart disease. My "inflammation and heart disease" and "angina" Theories explain why people develop heart disease and why this heart disease causes chest pain. In 2008 while developing a method to actually measure heart disease my research showed that changes in these blood tests of inflammation didn't match actual changes in heart disease; which means that measuring cholesterol and other blood tests won't tell you if your heart disease is changing. To know what's happening to your heart, you actually have to measure it. The only quantitative method for accurately, consistently and reproducibly being able to do this is FMTVDM. If the diet pundits want to know what happens to your heart when you go on their diets, they will need to measure it with FMTVDM.
FMTVDM; Breast cancer; Heart disease; Popular diets; Primary prevention; Secondary prevention
The recently accepted special report [1] from the American Heart Association (AHA) and the American College of Cardiology (ACC) makes recommendations regarding the primary prevention of atherosclerotic coronary artery disease (ASCAD); recommendations, which are based upon looking at various factors which are credited with causing the inflammatory process associated with ASCAD [2,3]. The primary author recognizes his responsibility in this debate as he is the creator of the “Inflammation and Heart Disease” and “Angina” Theories [2,3] is shown in Figure 1. It is therefore his responsibility to set the record straight. Not a record, which he incorrectly stated; but rather, a necessary correction after so many others have attempted to justify their positions based upon his “Inflammation and Heart Disease” and “Angina” Theories.
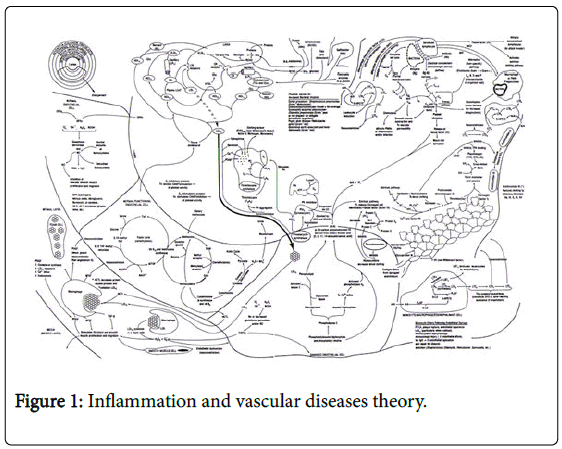
Figure 1: Inflammation and vascular diseases theory.
These markers of “Inflammation” include various contributing factors [2], which increase the risk of several chronic inflammatory diseases including but not limited to coronary artery disease (CAD), cancer, diabetes and hypertension. Depending upon which factors are elevated and the specific genetic responses of any given individual, the impact of each of these contributing factors varies. To merely measure them ignores this variability. The determination of the extent or change in the extent of disease (“Health-Spectrum”) must be directly measured (quantified) and not inferred or guesstimated from these surrogate blood markers [1-3]. Over the last several years multiple social media sites and medical journals have recruited opposing dietary pundit movements. Rather than focusing on the quantifiable end-organ outcome of the impact of these diets; clinicians, physicians, scientists and the lay public have allied themselves into factions focusing on supporting their beliefs rather than objectively measuring the true impact of their diets; viz. objective measurements of CAD and breast cancer. Up until recently, as will be discussed below [4], the objective measurement of these diseases was not possible. The motivation behind these “Diet Wars” appears to be for the same reason most wars occur; money, power, and prestige, and while this approach may work in politics, religion and the social media networks of the day; it has no place in Science or Healthcare.
The primary author joined the American Heart Association (AHA) in 1976 and joined the Physician Cholesterol Education Faculty shortly thereafter. Having taught and trained so many in Basic Cardiac Life Support (BCLS) and Advanced Cardiac Life Support (ACLS) I always smile when students are telling me about patients “risk factors” for heart disease, so it was no surprise to me when listening to a student talk about a woman who had just been admitted to the hospital the night before that the student ran down the list of “risk factors” for this woman. Yes, she was in her 40’s (age), but she was a woman (the number one cause of death in women is actually heart disease), without a family history of heart disease, she didn’t have high blood pressure, her cholesterol and lipid levels were all well below the acceptable levels for risk, she wasn’t overweight, she didn’t have diabetes, she exercised, she didn’t smoke. She didn’t appear to be a type A individual and she was following what at the time was considered a “heart healthy” diet only occasionally drinking alcohol.
After asking the student why he was running through all of these risk factors he replied it was important to know the patients risk factors because it helped determine her risk for heart disease. So what information could be drawn from her risk factors? Absolutely nothing. She had no risk factors for having a myocardial infarction (MI) yet this is exactly what had happened to her. Her electrocardiogram showed an inferior wall MI. It is this same guestimated inference being used by people to promote their diet regimens that can so easily mislead the general public and medicine itself. The “Inflammation and Heart Disease” Theory was an explanation of why CAD develops; not a call to measure these surrogate blood markers alone to determine treatment success or failure. This faulty incomplete reasoning is the driving force behind “The Diet Wars” now being waged upon the general public. There is such a desire to impress and be seen as right, that those involved are willing to do anything, except that which will discover the truth about the impact of these diets see “The Diet Wars Challenge” at the end of this article.
For many but not all people, the fundamental question is what is the actual impact of these diets on CAD and cancer. Studies looking at prevention and the outcome of diets, lifestyle, medications, medical procedures and surgery have focused on the impact these treatments have on various risk factors and surrogate blood markers defined in the “Inflammation and Heart Disease” Theory and not on actually measuring the resulting impact on CAD and Cancer itself. Many clinical tools commonly used; e.g. coronary arteriography, are now known to be flawed raising questions about what it means to truly “measure” CAD and Cancer.
After attending a recent Cardiovascular Conference and listening to discussions on “Artificial Intelligence” (AI), we are less convinced that people understand or are correctly using the term AI. Most of the discussion during this Conference focused on collecting larger and larger databases with information inferring the numbers of people having heart disease based upon “qualitative” imaging test results and surrogate markers of disease. The concept was to add all this information together to better guestimate the likelihood that someone has heart disease or breast cancer or whatever disease you were trying to find. This is nothing more than the accumulation of misinformation and mistakes under the pretense that this will somehow lead to a more accurate guestimate of disease by adding misinformation from a variety of sources.
This is also one of the problems present in large multi-center trials where variables, which while present at one institution, are absent at another. Such studies are a collection of multiple differences not defined but cumulatively necessary to provide enough participants to yield a statistically significant outcome that can be “published” owing to the miniscule difference that truly exists to begin with. True differences are statistically apparent in smaller studies resulting from the genuine statistical differences, which actually exist between treatment groups. The ability to find a statistical difference is either the result of a true statistical difference or there is no appreciable difference between treatment groups and only the inclusion of “massive” numbers of people in a study can make it look significant. You’ve heard the expression two wrongs don’t make a right; well such papers and proposed “AI” approaches would suggest that adding a lot of incorrect or partially correct information together including “qualitative” imaging tests which we know are flawed with “inattention blindness” and calibration errors, would somehow be an improvement. It’s just another set of “risk factors” being thrown into the mix of what has become a healthcare cauldron.
This is exactly what the medical student was trying to do with the woman. Putting the pieces together based upon what he expected to see and calling it probability; the probability that this woman had heart disease; except this probability didn’t represent an actual “quantitative” measurement upon which to place the probability. The AI frequently discussed now in the media and literature is nothing more than what the medical student was doing, only faster. In the end he was wrong as are these guestimates of heart disease and surrogate blood markers, which are being using to guestimate heart disease instead of actually quantitatively measuring it. Let us now turn our attention to the specific flaws of merely looking at Insulin Resistance, Cholesterol and Inflammation; beginning with Insulin Resistance, a term which people believe they are familiar with, but in reality are probably using and measuring, at least to an extent, incorrectly.
Insulin resistance
Insulin resistance is a term bandied about by many people today. It’s become a mantra for some people. There are a variety of ways people look for insulin resistance, including primarily surrogate blood tests. Many people have focused on looking at the ratio of triglycerides (TG) to high-density lipoprotein cholesterol (HDL); TG:HDL. This ratio is essentially the ratio of “fats” to “good cholesterol.” “Good cholesterol” (HDL) is a scavenger molecule of which there are actually three types depending upon how much they have been scavenging; HDL1, HDL2 and HDL3. This approach to “insulin resistance” became popular after it was noted that white overweight individuals with TG:HDL ratios greater than 3 were more likely to have “insulin resistance.” It is NOT however an actual measurement of Insulin Resistance; but a commonly used inference. Insulin resistance is a reference to diabetes mellitus and a more direct measure albeit still a blood test, is the use of glycosylated hemoglobin, also known as Hemoglobin A1C.
Too much insulin can be the result of inter alia a tumor, iatrogenic causes, or increased levels of caloric intake; primarily resulting from increased glucose and other sugars, frequently the direct consequence of refined carbohydrates. Simply replacing fats with refined carbohydrates as the food manufacturers did several decades ago, was clearly a marketing strategy and was never promoted by the medical community. Simply replacing saturated fats with refined carbohydrates or vice-versa, does not solve a problem, it merely exchanges one problem for another. This is a classic example of two wrongs don’t make a right. In fact, long before diabetes mellitus is present, we [5] showed (Figure 2) that even in the pre-diabetic range, there is an increased risk of vascular problems including cerebrovascular accidents (CVAs; aka “strokes) and transient ischemic attacks (TIAs; aka “mini strokes) occurring in Veterans. As shown in that study (Figure 2) individuals with higher blood glucose levels had a greater incidence of such vascular disease [5] long before they were considered to be “diabetic or insulin resistant.”
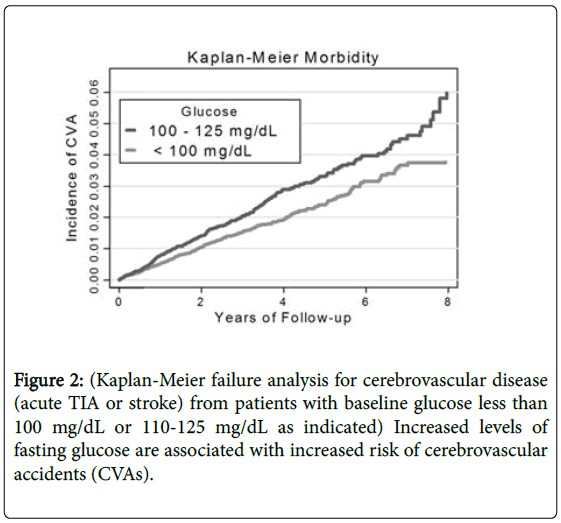
Figure 2: (Kaplan-Meier failure analysis for cerebrovascular disease (acute TIA or stroke) from patients with baseline glucose less than 100 mg/dL or 110-125 mg/dL as indicated) Increased levels of fasting glucose are associated with increased risk of cerebrovascular accidents (CVAs).
Furthermore, as already mentioned, HDL is nothing more than a scavenger mechanism. There are groups of people who have HDL’s in the 10-20 mg/dl range (considered very low) who have no heart disease attributed to their LDL levels being well below 60 mg/dl (again considered low) suggesting a “possible” species limit to significant CAD potential; even though this in and of itself does not “guarantee” the absence of disease in these individuals [2,3]; while still others have HDL’s in the 70-90 mg/dl range (considered high) who develop inflammatory plaques in their coronary arteries and go on to have heart attacks. There are still other individuals who have dysfunctional HDLs, dysfunctional to the extent that their production of HDL is increased in an attempt to compensate for the dysfunction, yet cannot do so due to the dysfunctionality of their HDLs. In fact, absent the A-1 Milano group, there is little if any scientific evidence that HDL does anything more than just movie the lipids (see below) around. What is insulin resistance and why the discussion? All food once ingested, be it protein, carbohydrate, alcohol of fat causes the release of insulin from specific cells in the pancreas called the islets of Langerhans. In fact, the term insulin actually comes from the Latin term, Insula, which means island. The major difference in insulin response by these various types of foods is how much insulin is released and how rapidly as shown in Figure 3. Simply put, the more refined the food, the faster the response. The higher caloric, the more sustained the response.
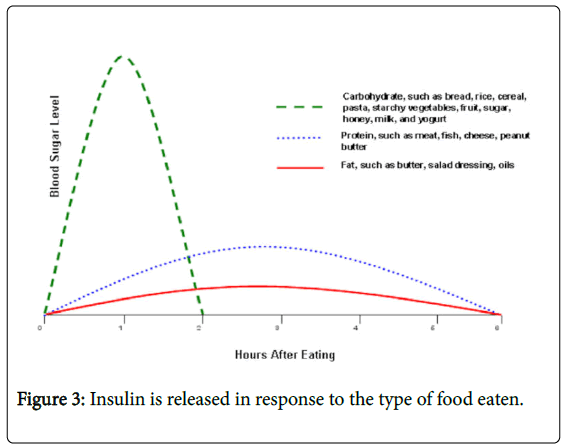
Figure 3: Insulin is released in response to the type of food eaten.
There is no question that the more elemental or refined the food is, the more rapidly the food will be broken down into its elemental components, independent of whether those food sources are plant or animal based. Once broken down these caloric sources as shown in Figure 4 are converted to acetyl coenzyme A within the cells of your body. This is subsequently converted into adenosine triphosphate (ATP) within the mitochondria of the cells of your body. ATP is the final energy source, which powers the cells of your body. Excess energy from the consumption of more food kilocalories (commonly referred to as calories) than required by your body is either stored in your liver as glycogen for more immediate needs or within other cells of your body as “fat” for future needs.
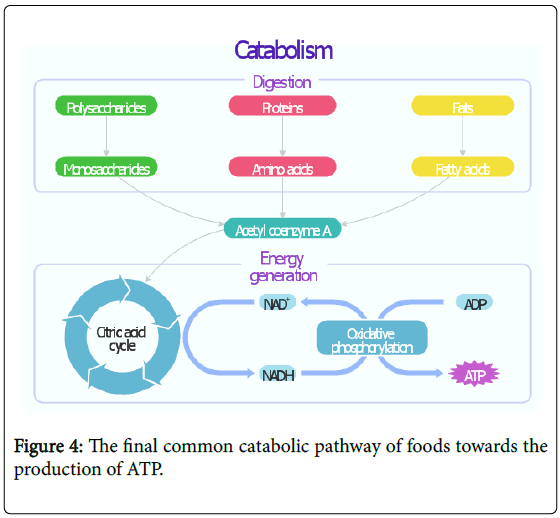
Figure 4: The final common catabolic pathway of foods towards the production of ATP.
As shown in Figure 5, glucose enters the cells of your body through the insulin receptors.
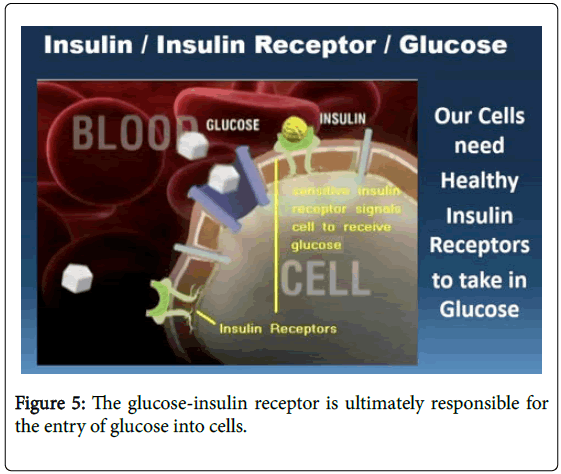
Figure 5: The glucose-insulin receptor is ultimately responsible for the entry of glucose into cells.
The cells within your body not only recognize how much glucose is in the blood stream but also how much is within the cells themselves. Under what we classically consider to be standard conditions, ours cells are in need of new energy (ATP) sources and are receptive to receiving more glucose from which to make the ATP. However, once the situation exists where the cells are no longer in need of energy sources and yet there are excess energy sources within the blood stream, the insulin receptors become less responsive; viz. “resistant.”
Insulin resistance means more and more insulin is required to stimulate these receptors, before the cells will allow more glucose to enter the cell. This process is termed “down regulation” of the insulin receptor and this is what “insulin resistance” truly is. The treatment for this insulin resistance is not merely the addition of more iatrogenic insulin or medications designed to increase insulin output by the pancreas, which only adds fuel to the fire of insulin resistance, but rather the reversal of this process. This is accomplished by decreasing caloric and glucose intake, resulting in less available glucose being made available to the cells, reducing cellular glucose and increasing the cellular need for glucose and energy substrates. Consequently increasing the cells insulin receptors responsiveness, the cellular uptake of glucose and the lowering of serum glucose levels with normalization of insulin receptor sensitivity.
Notice that the solution to the problem of insulin resistance (diabetes mellitus) is not merely switching from one type of food to another; viz. fat for carbohydrates, or carbohydrates for fat, but rather the overall reduction in caloric intake and refined processed carbohydrates, promoting an environment where the cells become insulin responsive, lowering insulin requirements, release and resulting health consequences.
Those who would argue to increase fat consumption in the place of carbohydrate consumption to address the problem are the same people who originally said it was wrong to switch fat consumption for excess carbohydrates; particularly refined carbohydrates. Simply switching one source of excess for another does not solve the underlying problem, it merely exchanges one set of problems for another. Those who argue that fat is the problem but have ignored or promoted increased carbohydrate, particularly refined carbohydrates intake in the place of fat have not solved the problem either; they have merely replaced one problem for another. Simply put, you don’t solve the problem of what you put in your mouth by putting something else in your mouth; you solve it by not putting the first thing in your mouth.
While it is true that the U.S. Military’s selection of Ancel Keys as its expert was simply the result of only having two people to choose from with high-altitude data on human caloric requirements, the initial observations about differences in death rates and what actually turns out to be “saturated” fat, no cholesterol per se, remain valid.
So too is the conscientious objector “confinement” data obtained by the U.S. Government during that same period of time, which determined the overall requirements and impact of calories, protein, carbohydrate and fat intake including the results of caloric and protein restrictions the U.S. Government imposed on these “participants” as the Government measured the consequential ability of these individuals to perform specific tasks; and the impact upon overall body weight and muscle mass, resulting from these “starvation” investigations. Our focus should be to learn not just from part of what we have learned, but to learn as much as possible from all the information acquired over the decades, including information gleaned at the expense of wrongful experimentation.
We’re really not talking about Cholesterol: We’re talking about lipids; the combination of cholesterol, fats and proteins combined. (Cholesterol=Lipid=lipoprtein levels) Cholesterol is a specific molecule, but when we talk about cholesterol in the blood stream, we are typically NOT referring to cholesterol itself, a hormonal precursor made in the adrenal gland but rather a combination of cholesterol, proteins and triglycerides (fats) [5]; collectively called lipoproteins or frequently shortened to lipids; these are commonly and incorrectly referred to as cholesterol.
This is one of the fundamental concepts needed to fully understand and appreciate that someone does not fully comprehend what they are talking about when they say cholesterol and saturated fat are not related to CAD. When someone refers to CAD as a problem with “insulin resistance” and then describes insulin resistance as the ratio of one lipid to another; viz. TG to HDL, they are by that very definition stating the problem is one of saturated fat. It is unconscionable to say lipids have nothing to do with heart disease and then to use the lipid levels to describe “insulin resistance” and say, this is what causes heart disease.
These different types of lipids include low-density lipoprotein cholesterol (LDL), intermediate density lipoprotein cholesterol (IDL), high-density lipoprotein cholesterol (HDL) of which there are as already mentioned essentially three types depending upon how saturated they are, very low density lipoprotein cholesterol (VLDL) and chylomicrons (essentially triglycerides; fats). These terms are based upon the original recognition of the various types of lipoproteins resulting from their separation in blood samples once centrifuged. That which settled to the bottom of the test tube was the densest, HDL, with LDL above that, IDL above that, VLDL above that, with chylomicrons being the least dense, floating to the top of the test tube. The greater the protein content, the greater the density; the greater the “fat” content, the lower the density.
When we speak of the liver producing “cholesterol” what we are actually saying is that the liver is making VLDL, which is mostly triglycerides (fat). Collectively, as shown in Table 1, these various lipids result in 6-different clinical types of lipid problems depending upon the specific type(s) of lipid abnormality we are talking about as shown in Table 1.
| Type | Disorder | Cause | Occurrence | Elevated plasma lipoprotein |
|---|---|---|---|---|
| I | Familial hyperchylomicronemia OR Primary hyperlipoproteinemia | Lipoprotein lipase deficiency OR Altered ApoC2 | Very rare | Chylomicrons |
| IIa | Familial hypercholesterolemia or Polygenic hypercholesterolemia | LDL receptor deficiency | Less common | LDL |
| IIb | Familial combined hyperlipidemia | Decreased LDL receptor | Commonest | LDL and VLDL |
| III | Familial dysbetalipoprotenemia | Defect in Apo E-2 synthesis and increased ApoB | Rare | IDL |
| IV | Familial hypertriglyceridemia | Increased VLDL production and decreased excretion | Common | LDL |
| V | Endogenous hypertriglyceridemia | Increased VLDL production and decreased Lipoprotein lipase | Less common | VLDL and chylomicrons |
Table 1: The classification of abnormal lipoprotein disorders.
The greatest limitation in simply measuring the different blood cholesterol lipid levels in the blood to assess the risk of heart disease for any given individual as we saw with our woman who presented to the hospital with an MI is [1] related to the individual differences (below) in how effectively any given individual metabolizes these lipids, something not measured with these surrogate blood tests and [2] the reality that these lipids which are associated with CAD exist primarily within the cells of the body and are not flowing freely through your bloodstream. It is within the cells of your body and within the walls of the coronary, carotid and other arteries of the body, not within the lumen of these blood vessels where the blood flows; where these “inflammatory” plaques result from the accumulation of lipoproteins and the other associated factors and inflammatory response [2,3], which will eventually rupture the arteries; leading to the real damage, viz. the final heart, brain, kidneys, liver and other end organ damage leading to morbidity or mortality.
In fact, roughly 85% of the body lipids, those that are actually causing the end organ damage of MI, CVA, CANCER and other inflammatory diseases, lie inside the cells proper. This is where the lipids reside and this is where they cannot be measured absent tissue biopsy of those organs to measure the internal cellular lipid levels. As this is both invasive and we have no real data to assist in the clinical decision making process using this approach, we are limited in the information serum lipids actually provides us.
This is just another reason why knowing the woman’s cholesterol level did not help the medical student in his assessing her risk for having heart disease. In fact, during conditions of “stress” and having a myocardial infarction (MI) would certainly qualify as a condition of stress, the blood epinephrine and cortisol levels increase; increasing your glucose levels and reducing your blood lipid levels; making the measurement of blood lipid and glucose levels during this period of time completely unreliable as markers of true “baseline” risk status.
Inflammation and heart disease
Unlike in 1999 when the primary author introduced the Theory of “Inflammation and Heart Disease” [2,3] and in 2000 introduced the “Angina” theory, showing that Angina [6-11] is actually caused by regional blood flow differences (RBFDs) and not simply the result of a narrowed coronary artery lumen, even though a narrowed coronary lumen can result in RBFDs; these Theories and concepts are now commonly accepted by most as our basis of Medicines understanding of both the cause of CAD and why angina occurs when someone has CAD; in addition to the inclusion of “measurement” of RBFDs and metabolic differences [5] in diagnosis and treatment of other diseases like Cancer. Included in the acceptance of these theories is the recognition that angina resulting from these RBFDs resulting from this “Inflammatory” process results in one of two types of MIs. The first, type I MI, resulting from the rupture of a vulnerable inflammatory plaque (VIP) with consequential thrombus formation and the second, type II MI, resulting from the RBFDs alone without plaque rupture. With type II MIs having a statistically significantly poorer survival that type I MI.
Despite the recognition and acceptance of both the “Angina” and “Inflammation and Heart Disease” Theories, there appears to be little true understanding of either theory, with Physicians continuing to measure the blood surrogate markers and define patients heart disease and other health problems based solely upon those surrogate “Inflammatory” Markers/Factors. Such clinicians presume these surrogate markers are actually measuring heart disease itself and treat their patient’s angina accordingly. They are not basing their treatment upon measurable differences in RBFDs.
It is almost impossible to pick up an article on “Inflammation and Heart Disease” and not see a cute little cartoon showing an artery on fire and while imitation may be considered to be a form of flattery, there are way too many people manipulating data and studies solely for the purpose of using the theory to support their positions; positions which demonstrate they do not fully understanding or appreciating the “Inflammation and heart disease” and “Angina” Theories. As such, it is not a compliment, it is not flattering and it does not promote or advance the understanding of inflammatory health care problems by misrepresenting the Theories; particularly when the components of the theories are being incorrectly explained and manipulated. Such actions MANDATE that the primary author respond to correct the literature almost 20-years later after the introduction of these Theories and to address the limitations in current studies, including Dietary outcome studies.
THE interaction between genes and environment
Biological systems are intricate and by that we mean they have evolved to provide a survival benefit, which includes responding to biological insults to keep the organism alive. They are not simple single gene responses and since much of the body’s inflammatory mechanism determines life or death, it has multiple complex backup systems to prevent death should one of the components fail to work adequately. Absent such a backup system only a single failure would be required and such a system would be biologically extinguished. Hence, such an organism with such a simplistic genetic makeup would undoubtedly already be extinct and we not concern ourselves with it.
These biological insults undoubtedly originally began with a combination of genetic and environmental factors initially beyond human control. Unsuccessful survival mechanisms lead to the extinction of those individuals with such inadequate genetic survival systems resulting in that genetic material no longer is being passed on. By contrast, successful response was evolutionarily rewarded by perpetuation through offspring and survival of the species. Over time, as humans have “evolved” (one can question whether this is such a good term considering the perpetuation of our chronic disease states and what appears to be a continual set of behaviors which appear determined to extinguish the species) we began to impact our environment(s) more and more; changing our living conditions, including reducing our need to physically perform manual labor tasks and the introduction of higher caloric sources of food, exceeding our biologic needs.
For over a hundred years, at least as far as modern humans are concerned, there has been considerable debate and discussion regarding those diseases most likely to kill us and why. Prior to the introduction of modern antimicrobial disease theory, therapy and antibiotics, by [1] Dr. Ignaz Semmelweis who had to endure the criticism and attacks of his “peers” only to be recognized for his significant contribution to medicine after his death and [2] Dr. (Sir) Alexander Fleming for his discovery of penicillin, the number one cause of death among people was infectious disease. Changes occurred during and around WWII, when increased caloric sources and lifestyle changes resulted in an increase in heart disease. During WWII itself with the institution of rationing, heart disease itself retreated, albeit only for a brief period of time.
By 1976, the primary author had joined the American Heart Association (AHA) and was soon on the Physician Cholesterol Education Faculty. The AHA had taken the position that based upon Ancel Keys and the work of others including certain epidemiologic information, that it appeared that cholesterol was the primary cause of heart disease. The current recommendations [1] demonstrate no deviation from this position.
Measuring heart disease means measuring heart disease not merely checking surrogate markers/blood tests
During the past four decades while the primary author completed his medical training and participated in several studies on the impact of diet and heart disease, including working on the dietary studies of others, as well as his own studies including some with the co-authors of this paper, it became apparent that valuable pieces of information were missing. Consequently the development of the “Inflammation and Heart Disease” and “Angina” Theories evolved and a recognition that merely measuring these surrogate blood tests/factors cannot satisfactorily measure whether changes in CAD or Cancer are resulting from such dietary regimens/treatments.
The primary author who began working with the Physician Cholesterol Education Faculty several decades ago has evolved his work and understanding into the Fleming Unified Theory of Vascular Disease (FUTVD) or if you prefer the name it is better known by, the “Inflammation and Heart Disease” Theory (©1-655833842, TX-7-451-244), which included LDL; VLDL; HDL; TG; weight; homocysteine; lipoprotein(a); fibrinogen; growth factors including insulin; interleukins; exercise; the complement cascade system; bacteria, viral, fungal and other infections; and antioxidants to name just a few of the components. The Theory considered the implications and effect of these and other various factors as they related to Heart Disease, Cancer, Diabetes, Hypertension and a number of other Chronic Inflammatory Processes.
The end result was a recognition that these multiple factors account for approximately 67% of the impact upon these diseases but more importantly, the recognition that any given individual has a unique biologic set of factors, and it is the individual’s specific response to those factors, which determines the final outcome; a final outcome which is not measured simply by measuring these surrogate blood tests/factors.While investigating [11] changes in these various surrogate blood factors/markers and comparing the changes in these factors over time, with changes seen in ischemic index (II) of coronary blood flow; the semi-quantitative measurement of coronary artery disease available at the time and the predecessor of the first quantifiable measurement of CAD and Cancer [4].
The results showed there was no relationship between the actual measured surrogate blood tests/factors, which are responsible for ultimately producing the inflammatory changes and plaques, with the end result of impaired coronary RBFDs, resulting from the inflammatory plaques. This is demonstrated in Figure 6 [12].
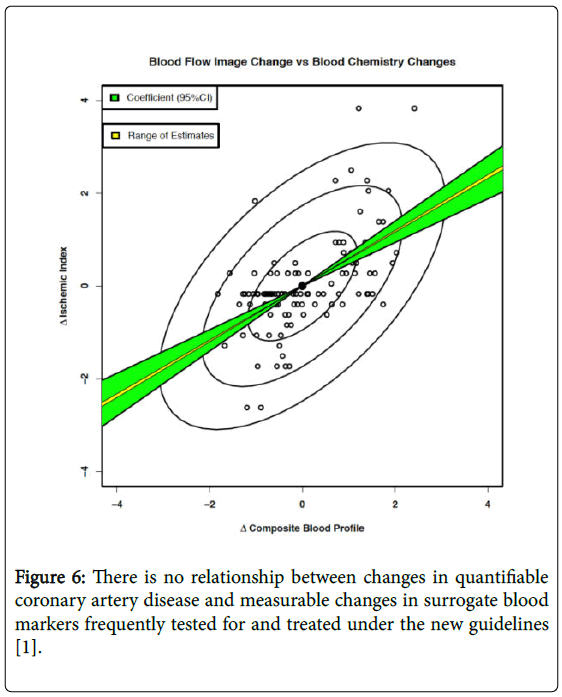
Figure 6: There is no relationship between changes in quantifiable coronary artery disease and measurable changes in surrogate blood markers frequently tested for and treated under the new guidelines [1].
It is in fact the final outcome of RBFDs and not the measurement of any one or more combination of these factors, which is the most important question to answer when asking if there is CAD, Breast Cancer or any other particular health problem and whether treatment has improved or worsened that problem having recognized this as a significant limitation by the late 1990s.
The primary author began working on the development of a truly quantitative artificial intelligence (AI) method for measuring the final outcome of these inflammatory diseases [4] by providing an absolute quantification of RBFD and metabolic differences in tissue; through equipment calibration, quantification and theranostification. A test, which not only accurately, consistently and reproducibly measures what is being looking for, RBFDs and metabolism, but also importantly a test without qualitative human errors, including “inattention blindness”, data loss and reader bias.
Why all dietary studies to date are flawed?
For decades we have been modifying the foods people consume and wondering about the affect these foods might have on the overall health of people. It is thought that obesity resulting from our increase caloric intake and our decreased caloric output (physical exertion) is now the major contributor to our incidence of Heart Disease, Cancer, Diabetes Mellitus and multiple other chronic inflammatory processes. How we have gotten to that state is one of debate.
Studies, which have looked at the various surrogate markers detailed in the “Inflammation and Heart Disease” and “Angina” Theories have failed to lead to helpful conclusions. The reasons now should be obvious to the reader. It is not a flaw in the Theories but rather a misapplication of the theories failing to recognize the full meaning, application and implications of the Theories and the work, which went into developing them. Like many other problems present in today’s society, there are major opposing polarized groups each insisting they have the answer, while claiming the other extreme has produced the problem. It is impossible with today’s “social media” to avoid the onslaught of articles, some scientific, many not so much, supporting each position. None of these articles however actually measure or quantify the diseases in question; viz. CAD and Breast Cancer. Neither do they measure the actual treatment effects of these diets upon CAD or Breast Cancer.
A classic example shown in Figure 7 shows how using FMTVDM, the Breast Cancer Imaging Component (B.E.S.T.), actually measures the affect of soy protein in two different women. In the first instance (left panel) the women showed measureable improvement in her breast health while in another women (right panel) the soy product measured a worsening of breast health. It is this quantification of outcomes that is badly needed to answer the question, what impact do these diets have on both Heart Disease and Breast Cancer.
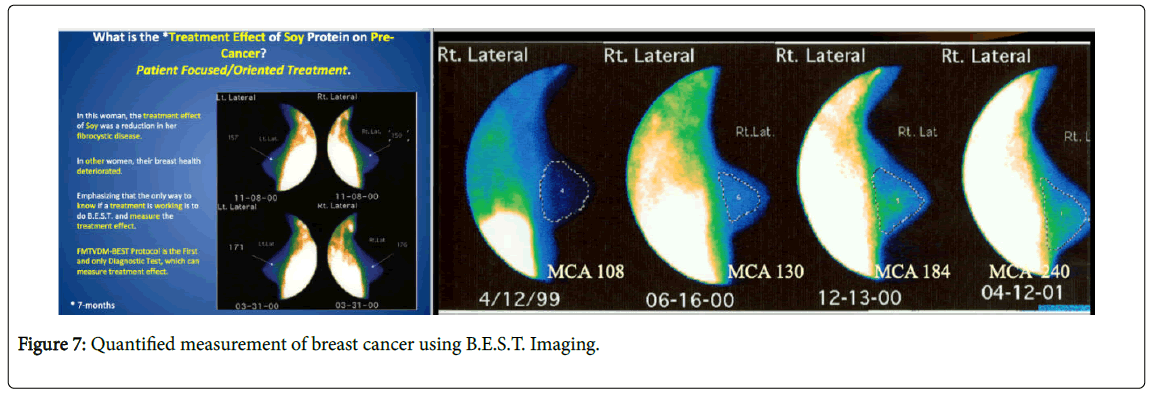
Figure 7: Quantified measurement of breast cancer using B.E.S.T. Imaging.
Due to the lack of quantifiable end organ outcome information (Heart Disease, Breast Cancer), the results of the myriad of diet studies have depended upon the less than completely reliable qualitative imaging studies, and the measurement of surrogate blood markers/ factors and changes in weight; none of which answer the question and merely add fuel to the fire of “The Diet Debate” while failing to quench the fire of inflammation responsible for heart disease and breast cancer plaguing modern societies.
The diet wars challenge: A time to measure the consequences resulting from popular diets
Our most recent publication [13,14] raised the question as to the validity of conducting studies without this quantitative [4,11] measurement. The studies [13,14] clearly demonstrate the ability of people to following dietary changes for longer periods of time then previously thought possible, provided there is appropriate dietary counseling, which in our studies included Bandura self-efficacy counseling. One of the common complaints in almost every, if not every, diet study is a question of experimenter bias; usually raised by the dietary pundits most adversely affected by the results. Those who have any publications to date have already drawn some conclusions but those conclusions as mentioned are severely limited by the outcome measures of qualitative imaging, weight loss and the measurement of surrogate blood markers which as has been noted above, does not show the actual quantitative changes in Heart Disease or Breast Cancer which truly occur.
Coupled with the ever-present concern that those conducting the dietary arms of many of the published and unpublished studies are undoubtedly not doing as good a job of instructing individuals on the diet as those who “believe” in the diet, it is important that such a quantitative study be done with the dietary arms of the study to be carried out under the direct supervision and control of those who are ardent proponents of each given dietary regimen; thereby removing this as a concern. To that end it is very clear that if we are to get to the bottom of this diet debate, if we are to truly determine what impact these diets are having on true disease outcomes, then we need a prospective dietary study, where the diet pundits in the respective camps become responsible for instructing and monitoring the activities of their participants. If no one can conduct a proposed dietary philosophy as well as those who worship at the alters of that diet, then they should and must be the ones to control and subsequently be responsible for writing up and living with the results of the study. Each group should measure the same outcomes. If they wish to measure weight, BMI, the surrogate blood markers, urinary ketones, respiratory quotients, whatever they want to obtain information on, they should do so, but all dietary groups should measure the same thing, so results can be compared between groups once the study is completed. The only requirement is that all participants, independent of what dietary group they are following must undergo FMTVDM & B.E.S.T. Imaging [4] to provide truly quantitative data as to the extent of heart disease and breast disease, both before and after the study. No other treatment regimens are allowed, to avoid contamination of outcome data. Since FMTVDM;B.E.S.T. Imaging is the only patented AI truly quantitative study, which measures changes in RBFD and metabolism, which by definition defines CAD and breast cancer, not only does FMTVDM provide the needed quantification to measure outcomes, but the results cannot be changed or modified through investigator intervention or manipulation.
As a patented study, it has been approved and most recently recognized by the American Society of Nuclear Cardiologists (ASNC) at the 2018 Conference (Figure 8) and in multiple other peer-reviewed medical journals [15-17]. The “Diet Wars Challenge” study should be initiated following an Initial media release specifying that the study is being initiated and stipulating, which diets are being included in the study and which diets are either not included or have elected not to participate. The inference is obvious. If you believe your dietary regimen is the answer to the question, then you would certainly want to participate. You will be less interested in participating if you are not so confident. Such a public press conference and/or media release of information will also make it crystal clear, not only which groups are participating but a similar press conference and/or media release will occur following completion of the study to discuss the results. The primary authors participation in the study will only be the quantification of Heart Disease and Breast Cancer Imaging using FMTVDM; FMTVDM-B.E.S.T. He will not be conducting a dietary arm of the study, nor will he endorse one of the dietary arms of the study.

Figure 8: Absolute quantification of CAD using FMTVDM.
What we have supported for dietary changes up to this point primarily include caloric control as well as limiting both saturated fats and refined carbohydrates as we consider these to be proinflammatory dietary influences. The primary authors only focus in this study will be to provide the only truly quantitative outcome measurements available for measuring CAD and breast disease through the measurement of RBFDs and metabolism [4]. All data results will be redacted of personal identifying information and will be made publically available. All dietary groups must agree to this at the outset to be considered for inclusion in the study. There will be no exceptions and no deletion of results. In the end, this will be the first dietary study providing real quantitative information about CAD and breast cancer, leaving no doubt about the affect of dietary intervention, data validity or final outcomes. The results will first be released through the same media source, originally used to make the public aware of the study, with others being able to provide results in tandem.
What do we believe?
We include this at the end of The Fleming Diet Challenge to address what is undoubtedly a point of interest by many; what is the motivation? During the past few decades, we have had the opportunity to publish papers, give presentations, listen to others, and like so many of you, consider the questions being pondered about inter alia diets, heart disease and cancer. We have looked at a variety of diets over decades; the claims that have been made, the outcomes reported; just as the primary author did during his reflection and development of the “Inflammation and Heart Disease” and “Angina” Theories. To find the truth frequently means looking outside one’s comfort zone or current knowledge base. This is true for everyone involved in investigating heart disease and cancer and working towards advancing the understanding and treatment of these diseases.
Here is what we believe! We believe that many people have some epidemiologic information or case studies, which have caused them to believe in a certain approach to eating. We also believe that others simply have a preference for certain foods and are looking to support their preferences as the right foods to eat. We believe that a number of people probably began with the right intentions and motivation for answering the question of which foods are good for you, which are bad for you and which have no substantial impact at all. We also believe the food industry is motivated by profit and will do whatever it needs to do to remain so. These corporations have already demonstrated this over the years, by increasing the numbers of highly refined and trans saturated fat foods available for consumers. Intriguingly enough these changes have extended the shelf life of foods while quite probably reducing the “shelf ” life of people. Independent of what the current dietary trend is, the food industry will switch to the production of those foods necessary for the food industry to continue to make a profit. To be crystal clear, the food industry in this instance does NOT include the farmers and ranchers growing the food and much of what is currently consumed, can only loosely be called “food” at least to someone raised in Iowa, who came from farm families.
We also believe the U.S. Government is more focused on dealing with surpluses it has and is more interested in distributing those surpluses as a means of justifying policy decisions that have been made, than it is about the overall health of society. If we have learned anything, it may be that there is more money in disease than health; at least up to the present models. We additionally believe that many of the people focused on promoting a certain type of diet have lost the perspective they once had. Motivational factors of proving oneself right or continuing to receive the financial benefit of diets being promoted, have tainted objectivity and obscured the final benefit awaiting people once objective measurements of outcomes of these diets have been made; measurements which we am calling for in this “Diet Wars Challenge”. What do we believe? We believe we indisputably need to get back to science and objectively measure the affect these diets have on Heart Disease and Breast Cancer and we stand ready to find that answer with your help. That’s what we believe!
Citation: Fleming RM, Fleming MR, McKusick A, et al. (2019) A Call for the Definitive Diet Study to End the Diet Debate Once And For All. Gen Med (Los Angeles) 7:322 doi: 10.35248/2327-5146.7.322
Received: 20-Mar-2019 Published: 17-Feb-2019, DOI: 10.35248/2327-5146.7.322
Copyright: © 2019 Fleming RM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.