PMC/PubMed Indexed Articles
Indexed In
- Open J Gate
- Genamics JournalSeek
- JournalTOCs
- Ulrich's Periodicals Directory
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- Proquest Summons
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
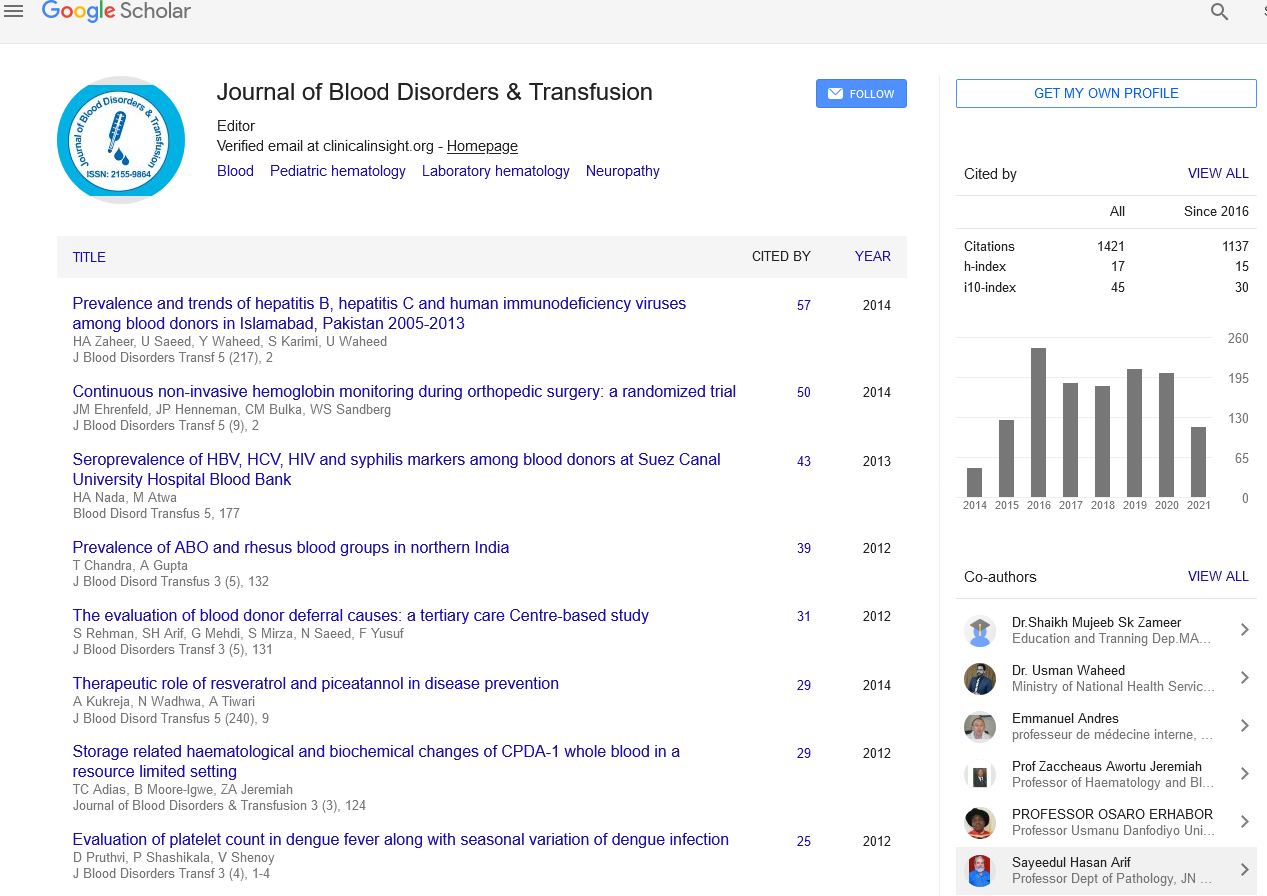
- Google Scholar
Useful Links
Share This Page
Journal Flyer

Open Access Journals
- Agri and Aquaculture
- Biochemistry
- Bioinformatics & Systems Biology
- Business & Management
- Chemistry
- Clinical Sciences
- Engineering
- Food & Nutrition
- General Science
- Genetics & Molecular Biology
- Immunology & Microbiology
- Medical Sciences
- Neuroscience & Psychology
- Nursing & Health Care
- Pharmaceutical Sciences
Abstract
A case of uterine adenomyosis that led to the rapid development of blood coagulation disorder two days after an induced abortion
Nishimoto M, Fujioka T, Saito M, Saito S, Kurakata M, Sugawara J, Yaegashi N and Sugiyama T
Cases of uterine adenomyosis in which disseminated intravascular coagulation is rapidly induced by infection, surgery, fertility treatment, abortion, or delivery are occasionally reported, but little is known about these conditions. We encountered a case of uterine adenomyosis in which the patient developed a rapid blood coagulation disorder 2 days after curettage for a missed abortion. A 39-year-old Japanese woman visited a private clinic with secondary amenorrhea, and was found to be 11 weeks pregnant. Three days later, she was diagnosed with missed abortion, and was transferred to our hospital with severe abdominal pain the day after the curettage. She complained of lower abdominal pain and pains from the hips to both lower extremities. Transvaginal ultrasonography revealed a diffuse uterine adenomyosis in the posterior uterine wall, and no remaining fetal tissue was visible in the uterine cavity. Laboratory findings at admission showed only mild elevation of WBC count, however, D-dimer and fibrin degradation product levels were abnormally high. After hospitalization the symptoms improved with nonsteroidal anti-inflammatory drugs, and the laboratory findings obtained the next day revealed a marked blood coagulation disorder, deteriorating renal function, decreased platelet count, and increased Lactate Dehydrogenase (LDH) concentration. No apparent thrombosis was observed on CT, and MRI revealed diffuse uterine adenomyosis in the posterior uterine wall with an irregular high intensity area. She was diagnosed with microthrombosis in uterine adenomyosis, and a total hysterectomy was performed. Surgical findings showed mild endometriosis adhesion in the dorsal uterus. Villous components were confirmed in the uterine cavity. Histopathology showed diffuse hemorrhage in the interstitium of the uterine adenomyosis and fibrin thrombus formation. The patient was diagnosed with intratumoral thrombosis caused by uterine adenomyosis. The patient’s blood coagulation disorder and deteriorating renal function improved gradually after surgery. The patient made steady progress, and was discharged 10 days after surgery.
Published Date: 2019-05-27; Received Date: 2019-05-04